Case Report
Sneddon -Wilkinson Disease: A Neutrophilic Autoinflammatory Disorder
1 Third-year resident physician, postgraduate dermatology program, University of Carabobo. Venezuela.
2 Dermatologist, Master in Educational Research. Postgraduate Professor of Dermatology, University of Carabobo. Coordinator of the Postgraduate Program in Dermatology, University of Carabobo. Attending Physician, Dermatology Service, Dr. Enrique Tejera University Hospital. Venezuela.
3 Head of Service and coordinator of the Postgraduate Program in Dermatology, “Dr. Enrique Tejera” Hospital City, Faculty of Health Sciences, University of Carabobo, Valencia, Venezuela.
*Corresponding Author: Katherin Mejía,Third-year resident physician, postgraduate dermatology program, University of Carabobo. Venezuela.
Citation: Mejía K., Endara M., Vivas S., (2026). Sneddon -Wilkinson Disease: A Neutrophilic Autoinflammatory Disorder. International Journal of Medical Case Reports and Reviews, BioRes Scientia Publishers. 6(1):1-3. DOI: 10.59657/2837-8172.brs.26.087
Copyright: © 2026 Katherin Mejía, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: February 20, 2026 | Accepted: March 06, 2026 | Published: March 13, 2026
Abstract
Sneddon-Wilkinson disease is a rare, recurrent, benign pustular dermatosis that predominantly affects women between the ages of 40 and 70. It is characterized by hypopyon-like pustules located in proximal areas. The case described here involves a male patient with significant metabolic comorbidities and an atypical lesion distribution, representing a significant deviation from the classic epidemiological profile and constituting a relevant clinical finding.
Keywords: sneddon-wilkinson disease; patient; neutrophilic autoinflammatory disorder
Introduction
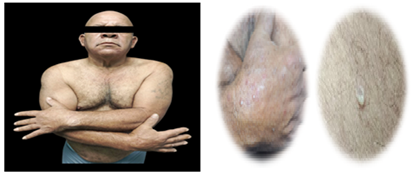
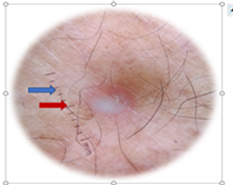
This is a 62-year-old male patient from the state of Carabobo - Venezuela, with a history of type 2 diabetes mellitus. He reports the onset of his current illness in 2024, characterized by pustules on the back of his hands, trunk, and lower limbs. He consulted multiple doctors who prescribed antibiotic therapy without improvement, and due to the persistence of the symptoms, he decided to visit the dermatology service in March of this year. On physical examination, the patient presented with skin phototype III and a generalized, bilateral, and symmetrical dermatosis, predominantly affecting the upper extremities. The lesions were characterized by a hypopyon-like pustule with an erythematous base, varying in size and distribution, and mild pruritus. The following presumptive diagnoses were considered: Sneddon -Wilkinson disease. Dermatoscopy revealed a superficial pustule and surrounding erythema with fine scaling at the periphery. Laboratory tests showed neutrophilia and hyperglycemia. A Gram stain was performed , revealing abundant neutrophils and negative bacteria. The patient was evaluated by the Endocrinology service, which also diagnosed grade II obesity. In a histological slide of skin stained with hematoxylin and eosin (H&E) and magnified 10X, subcorneal accumulation of neutrophils is observed in the absence of spongiosis and acantholysis. A superficial perivascular lymphohistiocytic inflammatory infiltrate is evident in the dermis. Based on the clinical and histopathological findings, a definitive diagnosis of Sneddon -Wilkinson disease is established. Systemic treatment with dapsone 100 mg/ day and prednisone 1 mg/kg/ day is initiated, and topical treatment with high-potency steroids is also prescribed. With favorable evolution at 6 weeks.
Figure 1: Hypopyon pustules on the back of the hands
Figure 2: Dermoscopy shows a pustule with an erythematous base
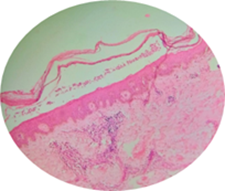
Figure 3: Histological slide of skin stained with H&E and magnified at 10X: Subcorneal accumulation of neutrophils is observed in the absence of spongiosis and acantholysis. In the dermis, a superficial perivascular lymphohistiocytic inflammatory infiltrate is evidente.
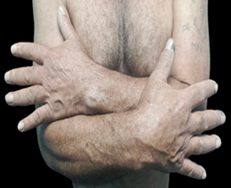
Figure 4: Remission of lesions 6 weeks after starting treatment with dapsone.
Discussion
Sneddon -Wilkinson disease is a rare, recurrent, benign pustular dermatosis that predominantly affects women between the ages of 40 and 70. It is characterized by hypopyon-like pustules located in proximal areas. The case described here involves a male patient with significant metabolic comorbidities and an atypical lesion distribution, representing a significant deviation from the classic epidemiological profile and constituting a relevant clinical finding. From a pathophysiological standpoint, this atypical form is related to its autoinflammatory neutrophilic nature, mediated by IL-8 and tumor necrosis factor-alpha, which is exacerbated in metabolic comorbidities such as diabetes mellitus. The absence of autoantibodies and positive cultures guides treatment toward neutrophil modulation. Dapsone is one such treatment. The therapy of choice , due to its direct action on neutrophils and its rapid clinical response, however, in refractory cases, therapeutic alternatives such as biological agents have been explored, thus expanding the therapeutic spectrum.
Conclusion
The identification of pustules in hypopyon constitutes a distinctive morphological marker that guides the diagnosis towards Sneddon -Wilkinson disease, allowing its differentiation from other neutrophilic pustuloses.Dapsone remains the conventional treatment of choice due to its effectiveness in inhibiting neutrophilic chemotaxis and its established therapeutic profile.
Summary
Sneddon -Wilkinson disease is a rare, recurrent, benign pustular dermatosis that predominantly affects women between the ages of 40 and 70. It is characterized by hypopyon-like pustules located in proximal areas. The case described here involves a male patient with significant metabolic comorbidities and an atypical lesion distribution, representing a significant deviation from the classic epidemiological profile and constituting a relevant clinical finding.
References
- Carrascosa JM, Gardeazábal J, Pérez- Ferriols A, Alomar A, Manrique P, et al., (2005). Consensus document on phototherapy: PUVA and narrowband UVB therapies. Actas Dermosifiliogr.,96(10):635–58.
Publisher | Google Scholor - Rodríguez R. (2015). Trimethoprim sulfamethoxazole. In: Academic Vademecum of Medicines. McGraw Hill.
Publisher | Google Scholor - (2015).Subcorneal pustular dermatosis or Sneddon -Wilkinson disease. Dermatol Rev Mex.,59(4):213–217.
Publisher | Google Scholor - Watts PJ, Khachemoune A. (2016). Subcorneal pustular dermatosis: a review of 30 years of progress . Am J Clin Dermatol.,17(6):653–671.
Publisher | Google Scholor - Valdés GJL, Solis CU, Valdés GEM, et al., (2016). Enfirmedad de Sneddon -Wilkinson. Rev Cuban Pediatrician,88(3):368–374.
Publisher | Google Scholor - Garcovich S, De Simone J, Berti E, Marzano AV. (2017). Drug management or neutrophilic dermatoses. Expert Rev Clin Pharmacol.,10(4):389–404.
Publisher | Google Scholor - May B, Hooper D, Mitty J. (2023). Trimethoprim -sulfamethoxazole: a general description.
Publisher | Google Scholor - Sánchez-González V, Morales-Cardona C, López- Takegami JCH. (2023). Pustular dermatosis Subcorneal : Eleven-year experience at a national referral center. Case report. Rev Association Colomb Dermatol.,36(2):267–277.
Publisher | Google Scholor - (2024). Sneddon -Wilkinson syndrome: a case report. Rev DCU.6(3):145–149.
Publisher | Google Scholor - Monteagudo Sánchez B. Diabetes and skin lesions. Rev Diabetes.
Publisher | Google Scholor - Calderón DC, et al. Diabetes mellitus and its different dermatological manifestations. Rev Colomb Endocrinol.
Publisher | Google Scholor - Carrascosa JM, Gardeazábal J, Pérez- Ferriols A, Alomar A, Manrique P, et al., (2005). Consensus document on phototherapy: PUVA and narrowband UVB therapies. Actas Dermosifiliogr.,96(10):635–58.
Publisher | Google Scholor - Rodríguez R. (2015). Trimethoprim sulfamethoxazole. In: Academic Vademecum of Medicines. McGraw Hill.
Publisher | Google Scholor - (2015).Subcorneal pustular dermatosis or Sneddon -Wilkinson disease. Dermatol Rev Mex.,59(4):213–217.
Publisher | Google Scholor - Watts PJ, Khachemoune A. (2016). Subcorneal pustular dermatosis: a review of 30 years of progress . Am J Clin Dermatol.,17(6):653–671.
Publisher | Google Scholor - Valdés GJL, Solis CU, Valdés GEM, et al., (2016). Enfirmedad de Sneddon -Wilkinson. Rev Cuban Pediatrician,88(3):368–374.
Publisher | Google Scholor - Garcovich S, De Simone J, Berti E, Marzano AV. (2017). Drug management or neutrophilic dermatoses. Expert Rev Clin Pharmacol.,10(4):389–404.
Publisher | Google Scholor - May B, Hooper D, Mitty J. (2023). Trimethoprim -sulfamethoxazole: a general description.
Publisher | Google Scholor - Sánchez-González V, Morales-Cardona C, López- Takegami JCH. (2023). Pustular dermatosis Subcorneal : Eleven-year experience at a national referral center. Case report. Rev Association Colomb Dermatol.,36(2):267–277.
Publisher | Google Scholor - (2024). Sneddon -Wilkinson syndrome: a case report. Rev DCU.6(3):145–149.
Publisher | Google Scholor - Monteagudo Sánchez B. Diabetes and skin lesions. Rev Diabetes.
Publisher | Google Scholor - Calderón DC, et al. Diabetes mellitus and its different dermatological manifestations. Rev Colomb Endocrinol.
Publisher | Google Scholor