Research Article
Efficacy of A Combination of Paracervical Block and Diclofenac Versus Pentazocine and Diclofenac in Pain Management During Manual Vacuum Aspiration, A Comparative Study
1Department of Obstetrics and Gynaecology, Usmanu Danfodiyo University Teaching Hospital Sokoto, Sokoto, Nigeria.
2Department of Obstetrics and Gynaecology Specialist Hospital Sokoto, Sokoto, Nigeria.
*Corresponding Author: Rabiu F. Anas, Department of Obstetrics and Gynaecology, Usmanu Danfodiyo University Teaching Hospital Sokoto, Sokoto, Nigeria.
Citation: Anas R F, Chukwuemeka N H, Mayana A, Mohammmed C A. (2025). Efficacy of A Combination of Paracervical Block and Diclofenac Versus Pentazocine and Diclofenac in Pain Management During Manual Vacuum Aspiration, A Comparative Study. Journal of Women Health Care and Gynecology, BioRes Scientia Publishers. 5(4):1-8. DOI: 10.59657/2993-0871.brs.25.083
Copyright: © 2025 Anas Rabiu Funtua, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: January 28, 2025 | Accepted: February 24, 2025 | Published: March 12, 2025
Abstract
Manual vacuum aspiration (MVA) is a surgical method of managing early pregnancy failure. It is a safe, effective, efficient and cost-effective technique. It is however associated with moderate to severe pain. The aim is to compare the efficacy of a combination of paracervical block and intramuscular diclofenac with intramuscular pentazocine and diclofenac in providing pain relief during the procedure. This was a randomized control trial that was conducted among women requiring MVA at the Gynaecological emergency unit of Usmanu Danfodiyo University Teaching Hospital (UDUTH) Sokoto. Patients were randomized into Group A offered Paracervical block and Diclofenac while group B were offered Pentazocine and Diclofenac. Their pain perception within 5-minute, 30 minute and 2 hours after uterine evacuation was assessed using the numerical rating scale (NRS), while the side effects profile were assessed using a questionnaire.120 patients were recruited. The mean pain score at 5-minute, 30 minute and 2 hours in group A were 2.55,0.43 and 0.03 respectively while that of group B were 6.43, 2.83 and 0.52 respectively and this was significant (p< 0.001). Side effect profile of dizziness, nausea and vomiting were better group A and as such patient were discharged earlier than in group B. About 80% of patient in group A had good satisfaction with the analgesia given and 90% will desire similar form of analgesia. These were found to be statistically significant p less than 0.001. Paracervical block plus diclofenac is an effective form of analgesia with lower pain score and better side effects profile.
Keywords: abortion; pain management; manual vacuum aspiration; paracervical block; diclofenac and pentazocine
Introduction
Early pregnancy failure is major public health concern worldwide [1]. It is defined as failure of a pregnancy before the age of viability. It is a common cause of maternal morbidity and mortality in most region of sub-Saharan Africa [2,3]. The aetiology of first trimester miscarriage is not known with certainty. However, chromosomal abnormalities have been implicated in about 50 – 80% of early miscarriages [4]. There are different modalities of treatment of an early abortion. These may depend on patient preference, clinical presentation and facilities available and protocol. These options include; expectant management, Medical and surgical management. Surgical management offers a faster approach than other methods, it is also the treatment of choice in actively bleeding patient, septic abortion, failed medical or expected management and molar gestation. Pain during manual vacuum aspiration is a major setback for patient undergoing surgical management. The sources of pain include from anxiety, cervical dilation and uterine evacuation and manipulation. As such pain management is an essential component of surgical management of miscarriages.
Various studies have attempted to identify the ideal method of pain relief during MVA with varying success in terms of pain relief, tolerable side effects and both patient and surgeon satisfaction. Some of the agents available for pain relief include non-steroidal anti-inflammatory drugs, opioids, local and topic analgesics, sedatives and anaesthetics [6]. These have been used either singly or in combination. No one agent has been found to be ideal for all patients [6]. Hence, essentially the highest level of satisfaction is achieved by providing the patient with various options of pain management so that she can choose a method that best fits her individual circumstances and wishes [7]. In my centers including mine, the combination of pentazocine and diclofenac is the recommended method of pain relief. This often cause sedation, vomiting and dizziness. This affect patient satisfaction, increase hospital stay and patients turn over, and work load to the health care provider and reduce availability of bed space. The aim of this study is to compare diclofenac and paracervical block with diclofenac and pentazocine in achieving pain relief and to also assess patient’s satisfaction.
Objective
To compare the efficacy of a combination of paracervical block and diclofenac with pentazocine and diclofenac in achieving pain relief during manual vacuum aspiration for first trimester abortion among women at Usmanu Danfodiyo University Teaching Hospital.
Methodology
This was a randomized controlled trial that compared the effectiveness of pain management during manual vacuum aspiration for the treatment of miscarriage between a combination of paracervical block and diclofenac versus pentazocine and diclofenac. The study was conducted on pregnant women that presented to Gynaecological emergency unit of the department with first trimester miscarriage and have an indication and consented for MVA. These group of patients include those with incomplete abortion, missed abortion, blighted ovum, and molar gestation. Those whose pregnancy is beyond first trimester, had septic abortion, sickle cell disease, allergic to any of the medications, chose other form of management and those that did not consent for the research were excluded. The patients were recruited in to the study by convenience sampling. They are then randomized in to two groups (A and B) using computer generated random numbers. Those in group A (study group) received standard dose of 75mg of intramuscular diclofenac and paracervical block with 15mls of 1% lignocaine while those in Group B (control) received intramuscular pentazocine 30mg and diclofenac 75mg within 10 minutes before the evacuation.
The evacuation was performed by IPAS trained doctors base on the standard IPAS procedure manual. Structured interviewer’s adminstred proforma was used at presentation to collect information on socio-demographic characteristics, medical and obstetric history of each participant. Gestational age was determined on best available estimate; either by using the patient’s last menstrual period or estimation of gestational age from a first trimester ultrasound scan. The pain scores at 5,30 and 120 minutes were taken after the procedure using the numerical rating scale (NRS). Then the observed and reported side effects were recoreded on the proforma. The sample size was calculated using the mean pain score of previous studies. The mean pain score where diclofenac and paracervical block was 5.0 and pentazocine and diclofenac was 4.2 and the estimated standard deviation was 1.5 [7].
Sample size for group comparison

Where n = sample size; Ϭ= Estimated standard deviation= 1.5; Z1-α/2= Z statistic for level of confidence of 95%= 1.96; Z1-β = Z statistic for 80% power = 0.842; µ1= Estimated mean pain score (large) = 5.0; µ2 = Estimated mean pain score (small) = 4.2; n = 55 .25 ~ 56 (Minimum sample size for each group)
An attrition rate of 5% was added. Hence 5% of 56 was 2.8. Total sample size rounded up to 60. Therefore, 60 women presenting with first trimester abortion were assigned randomly to group A (Paracervical block and Pentazocine) and another 60 women to group B (Pentazocine and Diclofenac) making a total of 120 women.
Intramuscular Diclofenac
The Diclofenac brand used was Diclofenac sodium 75 mg, marketed with the trade name Diclowin, with the batch number 230748; a product of Tianjin Chupet Pharm. Diclofenac was given IM into the upper outer quadrant of the left gluteus muscle, using a 23G hypodermic needle on a 5 ml syringe at a general dose of 75 mg. A latency period of about 10 minutes was allowed before the MVA was commenced to give room for the onset of analgesic action of the drug.
Pentazocine
The pentazocine brand was Fortwin manufactured by Sun pharmaceutical limited with a batch number HHA0010. It was given intra muscularly at 30mg stat on the alternate buttocks from the diclofenac in group B participant only.
Paracervical block
Patient was placed in lithotomy position under good light source. The cervix was exposed with a bivalve Cusco’s speculum. Tissue or blood clot around the cervical Os were removed. A 20mls syringe was used to withdraw 15mls of 1 % lignocaine and mounted on an 18gauge needle. About 2-3mls of lignocaine was injected at 12 o’clock on the cervix where the sponge holding forceps was placed. A slight traction on the cervix was applied to allow for easy visualization of the cervico-vaginal junction. About 3mls of 1% lignocaine was injected at 2, 4, 6 and 8 O’clock on the cervico- vaginal junction at a depth of about 2-3cm. At each injection site a gentle withdrawal of the plunger will be done to ensure the needle is not penetrating a blood vessel before injecting the anaesthetic drug. In both groups a period of about 10 minutes was allowed for the drugs to take effect before commencing the evacuation. Patients with missed abortion and a closed cervical Os were given 400ug of misoprostol per vaginum 4 hours prior to the evacuation to aid in cervical dilation.
Manual vacuum aspiration
Patient was placed in Lithotomy position. Perineum was cleaned with antiseptic solution and draped with sterile towels. The bladder was emptied. A bimanual pelvic examination is conducted. A Cusco’s speculum was introduced into the vagina and anterior lip of the cervix was held with Vulsellum to straighten the endocervical canal. Manual vacuum aspiration was performed with 60ml hand held Ipas MVA plus aspirator connected to an appropriate size Ipas easy grip canular. The procedure is done in the gynaecological emergency minor theater. A gentle evacuation was performed by slowly and gently rotating cannula and aspirator 180 degrees in each direction while using an in-and-out motion. This was continued until there was sign of emptying. Post evacuation the patient was assisted off the evacuation bed to a recovery room where her vital signs and pain assessment was carried out. Tissues evacuated were sent for histology. Vitals signs were monitored quarter hourly until patient was stable enough to be discharged. Patients were discharged on broad spectrum antibiotics and analgesia. Injection Anti D were given to unsensitized patients that were Rh D negative. Post abortal care was offered. They were counselled on signs of complications and where to present when they are noticed. A two-week appointment was given to present at the gynaecological clinic with histology result.
Pain assessment
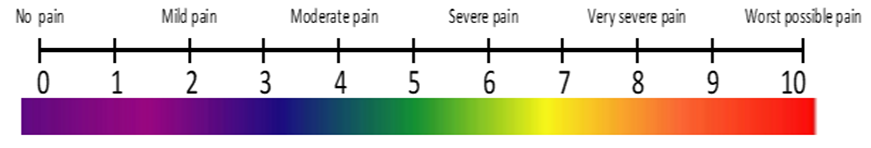
The numerical rating scale (NRS) for pain is a simple unidimensional measurement of pain intensity in individual. It consists of numeric values 0 – 10 in which respondents choose from based on the intensity of their pain. The values increase with increase pain intensity, with 0 being no pain and 10 the worst possible pain ever. It is a reliable and a reproducible tool for pain assessment [19]. There are no special skills required for either administrating, answering or interpreting it. Because of the aforementioned advantages, this tool was used for this study.
Patient assessment
The vital signs and pain assessment were conducted in the recovery room by the attending nurse who was blinded by the type of analgesia offered to the patient. The numeric rating pain scale was used to assess pain level and intensity. Individual patients were assessed immediately post operation (I.e., within the first 5 minute), 30 minute later and 2 hours later. While level of satisfaction was assessed and graded using the Likert scale.
Ethical issues
The research approval was obtained by the ethical research committee of UDUTH.
Data analysis
The data obtained was analysed using the IBM statistical package for the social sciences (SPSS) version 20. Categorical variables were summarized in frequencies and percentages. The mean pain scores within 5 minutes, 30 minutes and 2 hours were determined and compared among the 2 groups using the independent student t test and also represented on a line chart. While the median pain scores were compared among the different analgesic groups using the Mann Whitney U test. At a confidence interval of 95% and level of significance of 0.05. The comparison of side effects and patient satisfaction including desire for similar analgesia was made using chi square/fisher exact. Other information was summarized in a tables and figures.
Results
The 120 set of participants were randomized into the group A consisting of 60 participants (Paracervical group) and group B consisting of 60 participants (Pentazocine group). The Sociodemographic characteristics of respondents was summarized in table 1 and there was no significant statistical deference among the 2 groups.
Table 1: Socio-demography, indications for manual vacuum aspiration and biological characteristics of the participants
| Characteristics | Paracervical + Diclofenac group n (%) | Pentazocine + Diclofenac group n (%) | χ2 / fisher exact | P value |
| Age (Years) | 1.948 | 0.745 | ||
| Less than 20 | 4 (6.7) | 1 (1.7) | ||
| 20 – 24 | 11 (18.3) | 11 (18.3) | ||
| 25 – 29 | 16 (26.7) | 16 (26.7) | ||
| 30 – 34 | 10 (16.7) | 11 (18.3) | ||
| ≥ 35 | 19 (31.7) | 21 (35) | ||
| Ethinicity | ||||
| Hausa/ Fulani | 44 (73.3) | 43 (71.7) | 4.726 | 0.193 |
| Igbo | 6 (10) | 6 (10) | ||
| Yoruba | 9 (15) | 5(8.3) | ||
| Others | 1 (1.7) | 6 (10) | ||
| Religion | 0.208 | 0.820 | ||
| Islam | 49 (81.7) | 47 (78.3) | ||
| Christian | 11 (18.3) | 13 (21.7) | ||
| Others | 0 (0) | 0 (0) | ||
| Education status of respondents | 23.489 | 0.71 | ||
| Primary | 3 (5) | 2 (3.3) | ||
| Secondary | 20 (33.3) | 19 (31.7) | ||
| Tertiary | 29 (48.3) | 30 (50) | ||
| No formal education | 8 (13.3) | 9 (15) | ||
| Education status of spouse | 11.962 | 0.840 | ||
| Primary | 1 (1.7) | 0 (0) | ||
| Secondary | 20 (33.3) | 19 (31.7) | ||
| Tertiary | 26 (43.3) | 28 (46.6) | ||
| No formal education | 13 (21.7) | 13 (21.7) | ||
| Occupation of respondents | 13.847 | 0.831 | ||
| House wife | 35 (58.3) | 34 (56.6) | ||
| Student | 1 (1.7) | 2 (3.3) | ||
| Civil servant | 14 (23.3) | 14 (23.3) | ||
| Business | 4 (6.6) | 5 (8.3) | ||
| Others | 6 (10) | 5 (8.3) | ||
| Occupation of spouse | 9.046 | 0.290 | ||
| Farmer | 5 (8.3) | 6 (10) | ||
| Civil servant | 35 (58.3) | 36 (60) | ||
| Business | 14 (23.7) | 16 (26.7) | ||
| Others | 6(13.3) | 2 (3.3) | ||
| Knowledge of LMP | 6.818 | 0.330 | ||
| Known | 5 (8.3) | 3 (5) | ||
| Unknown | 55 (91.7) | 57 (95) | ||
| History of miscarriage | 0.580 | 0.356 | ||
| Yes | 27 (45) | 24 (40) | ||
| No | 33 (55) | 36 (60) | ||
| History of MVA | 0.841 | 0.5 | ||
| Yes | 17 (28.3) | 18 (30) | ||
| No | 43 (71.7) | 42 (70) | ||
| Gravidity | 2.703 | 0.259 | ||
| Primigravida | 11 (18.3) | 11 (18.3) | ||
| Multigravida | 16 (26.7) | 24 (40) | ||
| Grandmultipara | 33 (55.0) | 24 (41.7) | ||
| Gestational age | 3.870 | 0.276 | ||
| Less than 6 | 1 (1.7) | 1 (1.7) | ||
| 6 – 8 | 31 (51.7) | 25 (41.7) | ||
| 9 – 11 | 15 (25) | 25 (41.7) | ||
| 12 | 13 (21.7) | 9 (15) | ||
| Types of miscarriage | ||||
| Incomplete | 49 (81.7) | 47 (8.4) | 9.804 | 0.075 |
| Missed | 6 (10) | 8 (13.3) | ||
| Blighted | 5 (8.3) | 5(8.3) |
Table 2: Comparison of pain score between the 2 analgesics group.
| Time | Paracervical + Diclofenac group Median (IQR) | Pentazocine + Diclofenac group Median (IQR) | Mann Whitney U test | P value |
| Within 5 minutes | 2 (1 - 3) | 6 (5 - 8) | 396.5 | Less than 0.001 |
| 30 minutes | 0 (0 - 0) | 3 (0 - 4) | 775 | Less than 0.001 |
| 2 hours | 0 (0 - 0) | 0 (0 - 0) | 1468 | 0.001 |
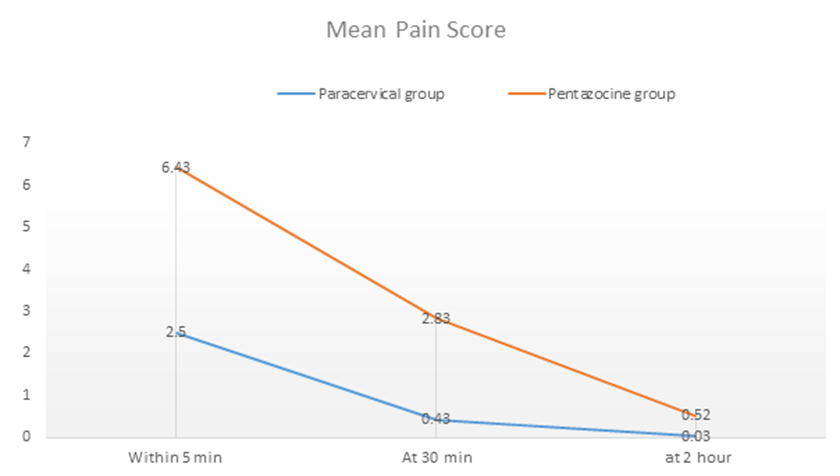
Figure 1: Pattern of mean pain scores across the duration of time assessed among the 2 groups
Table 3: Comparison for request of additional analgesia, satisfaction and desire for similar analgesia between the 2 groups.
| Variable | Paracervical block + Diclofenac group n (%) | Pentazocine + Diclofenac group n (%) | χ2 / Fischer exact | P value |
| Request for additional analgesia | 32.862 | Less than 0.001 | ||
| Yes | 4 (6.7) | 33 (55) | ||
| No | 56 (93.3) | 27 (45) | ||
| Satisfaction | 27.67 | Less than 0.001 | ||
| Good | 48 (80) | 22 (36.7) | ||
| Moderate | 9 (15) | 13 (21.7) | ||
| Poor | 3 (3) | 25 (41.7) | ||
| Desire for similar analgesia | 27.692 | Less than 0.001 | ||
| Yes | 54 (90) | 27 (45) | ||
| No | 6 (10) | 33 (55) |
Table 4: comparison of blood loss and time of discharge between the 2 groups.
| Variable | Paracervical block + Diclofenac group n (%) | Pentazocine + Diclofenac group n (%) | χ2 / Fischer exact | P value |
| Blood loss | 1.214 | 0.545 | ||
| Less than 50 | 30 (50) | 33 (55) | ||
| 50 – 100 | 29 (48.3) | 27 (45) | ||
| 101 – 150 | 0 (0) | 0 (0) | ||
| ˃ 150 | 1 (1.7) | 0 (0) | ||
| Time of discharge | 81.988 | Less than0.001 | ||
| Within 2 hours | 59 (98.3) | 10 (16.7) | ||
| 2 – 4 | 1 (1.7) | 20 (33.3) | ||
| 4 - 6 | 0 (0) | 30 (50) |
Table 5: Side effects profile between the 2 analgesics group
| Side effects | Paracervical + Diclofenac group n (%) | Pentazocine + Diclofenac group | χ2/Fisher exact | P value |
| Drowsiness | 26.44 | Less than 0.001 | ||
| Yes | 25(41.7) | 52 (86.7) | ||
| No | 35 (58.3) | 8 (13.3) | ||
| Nausea and Vomiting | 32.967 | Less than 0.001 | ||
| Yes | 6 (10) | 36 (60) | ||
| No | 54 (90) | 24 (40) | ||
| Dyspepsia | 0.120 | 0.500 | ||
| Yes | 4 (6.7) | 5 (8.3) | ||
| No | 56 (93.3) | 55 (91.7) | ||
| Tinnitus | 7.434 | 0.006 | ||
| Yes | 7 (11.7) | 0 (0) | ||
| No | 53 (88.3) | 60 (100) | ||
| Metallic taste | 1.534 | 0.151 | ||
| Yes | 13 (21.7) | 19 (31.7) | ||
| No | 47 (78.3) | 41 (68.3) | ||
| Numbness | 8.574 | 0.003 | ||
| Yes | 8 (13.3) | 0 (0) | ||
| No | 52 (86.7) | 60 (100) |
Discussion
The study aimed at comparing the analgesic effective of paracervical block and diclofenac versus pentazocine and diclofenac during manual aspiration for the surgical management of abortion. The age of respondents was between 18 – 48 years, with a mean age of 29.88 ± 6.77 and the modal class was 35 years and above. This is because the incidence of miscarriage increases with age. In fact, age is an independent risk factor for abortion [8]. Most of the respondents are grandmultiparae having 5 or more number of deliveries. This is not surprising as multiparity is a risk factor for miscarriage [9]. This is similar to studies in Kano, Abakaliki and Sokoto [3,10,11]. The modal gestation age at presentation was 6-8 weeks. This was similar to a study in Kano but lower than 10 – 12 found in Maiduguri and 8-12 in Abakaliki [2,10,11]. This is because majority of spontaneous abortion occurs in the first trimester [22]. The most common form of miscarriage in this study was incomplete abortion in both groups.
The mean pain score within the first 5 minute was 2.55 in the paracervical block group and 6.43 in the pentazocine group. There was statistical significance difference between the mean score of the paracervical group and pentazocine group with a p value of Less than 0.001. This implies that the paracervical group had a lower pain perception compared to the pentazocine group. The median pain relief within the first 5 minutes, 30 minute and 2 hours in the paracervical group were 2,0,0 and that of the pentazocine group were 6,3,0 respectively. The differences in the median pain scores were statistically significant in the first 5 minute and 30 minutes between the 2 groups (p = Less than 0.001). However, after 2 hours the pain score was the same (minimal to no pain) and this was found not to be statistically different between the two groups. This may be as a result of quick diminished MVA induced cramps, which usually occur within 30 – 60 minutes [12]. The pain perception was higher in the paracervical group (5.4) and lower in the Opioids group (Meperidine and Diclofenac) 5.0 in the study done in Panama by Lopez.13. The higher pain perception in the paracervical group in the study may be as a result of differences in ethnicity, geographical differences and biological makeup of the respondents. In addition, the Opioids group pain perception is lower because Meperidine is a stronger opioid than pentazocine. This may have further reduced the intensity of pain.
The request for an additional analgesia during the procedure was less (6.7%) in the paracervical group compared to the Pentazocine group (55%). Similarly, there was better patient satisfaction in the paracervical group than the pentazocine group. Most patient will desire paracervical block more than pentazocine. It will be logical to think this is because pain relief is better with paracervical compared to pentazocine group. These were all statistically significant with a p value of less than 0.001. Renner et al reported similar better patient satisfaction with paracervical group compared with sham [14]. However, Nishant et al reported a contrasting result, where patients that received deep sedation had a better satisfaction compared to those that received paracervical block [15]. A Cochrane review did not show any difference in terms of requirement for additional analgesia and patient satisfaction when paracervical block was compared with systemic analgesia and sedation [16]. Different methodology and study design coupled with study population may have accounted for the differences.
There was no statistical difference between the two groups in terms of blood loss. However, patients in the paracervical group were discharged earlier. About 98.3 percentage of respondents were discharged within 2 hours in the paracervical group and the remaining 1.7 Percentage within 4 hours. While only about 16.7 percentage of patients were discharged within 2 hours in the pentazocine group. Half of the respondent were discharged within 6 hours in the pentazocine group. The time of patient discharge was found to be statistically different between the 2 groups(p = Less than 0.001). This was as a result of dizziness, weakness and vomiting associated with patient under the pentazocine group.
Side effect such as drowsiness, nausea and vomiting were seen more with patient in the pentazocine group than the paracervical group. These differences were statistically significant with a p value of Less than 0.001. While, side effects such as numbness and tinnitus were seen more in the paracervical group and this was equally statistically significant p = 0.003 and 0.006 respectively. This again may be explained by the parenteral administration of pentazocine which may ultimately give more systemic side effect than locally administered paracervical block which has more action at the site where it was given. Side effects such as dyspepsia and metallic taste were not statistically different between the 2 groups. None of the respondents had cardio-respiratory depression, confusion or convulsion. In general, the fewer side effect found in this study is in keeping with the finding by the WHO and RCOG which resulted in the recommendation for its use for pain relief during manual vacuum aspiration [17,18].
Conclusion
Paracervical block using 1% lidocaine and intramuscular diclofenac during manual vacuum aspiration when compared to intramuscular pentazocine and diclofenac is a more effective method for pain relief. The side effects profile such as dizziness, nausea and vomiting were less in the paracervical group compared to the pentazocine group. As such, patients’ satisfaction and desire for similar form of analgesia is better with the paracervical block group. The use of paracervical block and diclofenac for pain relief is therefore a safer and more effective method of analgesia during manual vacuum evacuation when administered properly.
References
- Afshan A, Ayesha I. (2013). Effectiveness of manual vacuum aspiration in missed miscarriage of less than 12 weeks gestation. Journal of South Asia Federation of obstetrics and gynaecology, 5(3):154-157.
Publisher | Google Scholor - Isa B, Mairiga AG, Ibrahim SM, Bako BG, Usman HA. (2013). Experience with Manual Vacuum Aspiration at university of Maiduguri Teaching Hospital. Bo Med J, 10(2):31-35.
Publisher | Google Scholor - Garba JA, Nasir AM, Nwobodo EI, Tunau KA, Panti AA, Saidu AD, et al. Miscarriage in a tertiary health center in Northern Nigerin:a review of profile, causes and outcomes. Trop J Obstet & Gynaecl, 34(1).
Publisher | Google Scholor - Ann-Marie S, Samantha M. (2013). Early pregnancy risks. In: Alan H, Lauren N, Neri L, Ashley S, editors. Current Diagnosis and Treatment Obstetrics and Gynecology. New york: Mc Graw Hill, 234-249.
Publisher | Google Scholor - Davor J, Caroline O, Ruth B. (2013). Diagnosis and management of first trimeter miscarriage BMJ, 7.
Publisher | Google Scholor - Mirriam EW, Murray BA, Abbey J, Hardy FB, Adrianne RR, Colleen KS. (2014). Pain control options for first trimester surgical abortion: a review. proceeding in obstetrics and gynaecology, 4(2).
Publisher | Google Scholor - Natalia A, Galadanci H, Ibrahim S, Mohhammed Z. (2015). Comparison of effectiveness of pain management during manual vacuum aspiration using single agent analgesia and combination; A randomised double blind controlled trial. Open journal of obstetrics and gynaecology, 5:244-250.
Publisher | Google Scholor - Kamble G, Bhattacharya BM. (2017). Miscarriage and associated risk factors in India: a brief review. MOJ Womens Health, 4(4):84-86.
Publisher | Google Scholor - Adeniran A, Fawole A, Abdul I, Adesina K. (2015). Spontaneous abortions (miscarriages): Analysis of cases at a tertiary center in North Central Nigeria. Journal of Medicine in the Tropics, 17(1):22-26.
Publisher | Google Scholor - Anikwe C, Ikeoha C, Obuna J, Okorochukwu B, Nnadozie U. (2019). Five-year review of cases of miscarriage in a tertiary hospital in Abakaliki, South East, Nigeria. Tropical Journal of Obstetrics and Gynaecology, 36(3):367-372.
Publisher | Google Scholor - Idris UT, Habiba L, Usman AU, Attah RA, Zakari M. (2020). Manual Vacuum Aspiration in the Treatment of First Trimester Miscarriages: Experience from a Northern Nigerian Teaching Hospital. Jbcrs, 9(2):28-31.
Publisher | Google Scholor - Ireland LD, Allen RH. (2016). Pain Management for Gynecologic Procedures in the Office. Obstetrical & gynecological survey, 71(2):89-98.
Publisher | Google Scholor - Lopez JC, Vigil-De Gracia P, Vega-Malek JC, Ruiz E, Vergara V. (2007). A randomized comparison of different methods of analgesia in abortion using manual vacuum aspiration. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics, 99(2):91-94.
Publisher | Google Scholor - Regina M, Mark D, Jefferey T, Hong L, Alison B. (2012). Paracervical block for pain control in first trimester surgical abortion. Obstetrics and gynecology, 119:1037.
Publisher | Google Scholor - Sahay N, Agarwal M, Bara M, Raj N, Bhushan D. (2019). Deep Sedation or Paracervical Block for Daycare Gynecological Procedures: A Prospective, Comparative Study. Gynecology and minimally invasive therapy, 8(4):160-164.
Publisher | Google Scholor - Tangsiriwatthana T, Sangkomkamhang U, Lumbiganon P, Laopaiboon M. (2013). Paracervical local anaesthesia for cervical dilation and uterine intervensions. The Cochrane database of systematic reviews. 9.
Publisher | Google Scholor - (2006). Management of early pregnancy loss [Internet]. Royal college of obstetricians and gynaecologist.
Publisher | Google Scholor - (2014). ACOG. Medical management of first-trimester abortion. ACOG practice bulletin number, (143):1-18.
Publisher | Google Scholor - Hawker F, Samra M, Tetyana K, Meissa F. (2011). Measurement of adult pain. American College of Rheumatology, 63(11):252.
Publisher | Google Scholor