Review Article
Should We Give Azithromycin Prophylactically at Caesarean Delivery? Narrative Review
1Master’s Student in Medicine, University of Coimbra, Coimbra, Portugal.
2Faculty of Medicine, University of Coimbra, Coimbra, Portugal.
3ICBR Inflammation and Biomarkers Group, Coimbra, Portugal.
*Corresponding Author: Emília Oliveira Ginja, Master’s Student in Medicine, University of Coimbra, Coimbra, Portugal.
Citation: Ginja EO, Areia AL. (2026). Should We Give Azithromycin Prophylactically at Caesarean Delivery? Narrative Review, International Journal of Biomedical and Clinical Research, BioRes Scientia Publishers. 6(2):1-10. DOI: 10.59657/2997-6103.brs.26.112
Copyright: © 2026 Emília Oliveira Ginja, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: December 18, 2025 | Accepted: January 06, 2026 | Published: January 15, 2026
Abstract
Caesarean delivery rates have been increasing worldwide. With the rising frequency of this obstetric surgical procedure, there has been a parallel increase in associated complications, particularly infections. Although some measures have already been implemented to reduce infectious complications, namely standard antibiotic prophylaxis with 1g of intravenous cefazolin administered prior to skin incision, along with multiple aseptic measures, post-caesarean infections remain a significant concern. The main objective of this literature review is to identify scientific evidence on whether broadening the spectrum of prophylactic antimicrobial by combining azithromycin with a first-generation cephalosporin prior to Caesarean Delivery can reduce the incidence of post-caesarean infections. The references included in this review were obtained from Embase, Google Scholar, Medline, PubMed and Scopus databases. World Health Organization recommendations were reviewed and taken into account. Considering the mechanisms of action and spectra of activity of the above-mentioned antibiotics and the microorganisms most frequently implicated in surgical site infections following caesarean delivery, namely Ureaplasma spp. and Mycoplasma spp., it is proposed to broaden the prophylactic antibiotic spectrum by adding azithromycin as an adjuvant agent. Based on the scientific evidence currently available, it was concluded that the administration of 500 mg of intravenous azithromycin, in combination with the standard prophylactic regimen, may be beneficial in reducing post-caesarean infectious morbidity, including both endometritis and wound infections.
Keywords: macrolides; endometritis; caesarean section; surgical wound infection/prevention and control
Introduction
Caesarean Delivery (CD) is a surgical procedure involving the extraction of the fetus (alive or dead) and the placenta through incisions in the abdominal and uterine walls. It is an alternative to vaginal delivery that can prevent maternal and neonatal mortality [1]. Although it is associated with higher rates of maternal mortality and morbidity than a vaginal birth [2].
The caesarean section was first performed in the sixteenth century as a post-mortem attempt to save the life of a child whose mother had died. During the seventeenth and eighteenth centuries, the procedure was developed further and began to be performed on living mothers. At that time, there was a high mortality due to infections and maternal bleeding. In 1871, the first elective caesarean in which both mother and son survived was performed [3]. During the twentieth century, maternal mortality decreased significantly, reaching almost 1%, due to the advances in surgical technique with aseptic protocols, the availability of blood banks and access to antibiotics [2].
Since then, CD rates have been increased worldwide, becoming the most common surgical procedure performed on women [3].
To optimize the use of caesarean section, the World Health Organization (WHO) developed the Robson Classification. This is based on five criteria: parity, number of fetuses, fetal presentation, gestational age and onset of labor [4]. It regards every woman undergoing labor, to analyze and compare caesarean section rates across hospitals worldwide and to guide strategies aimed at reducing unnecessary CDs [5]. Ideally, a CD should only be performed when medically indicated, apart from prior caesarean section and failure to progress in labor, other evidence-based indications include malpresentation, cephalopelvic disproportion, abnormal placentation, multiple gestation and placental abruption [6,7].
The increasing number of CD is associated with an increase in complications arising from them, being infections one of the most common [6]. Indeed, the risk of postpartum infection is five to twenty times higher compared to vaginal birth. Among infections, the most common are surgical site infections (SSI), including wound infection and endometritis, both of which can lead to maternal sepsis [8-10].
Prophylactic antimicrobial therapy is widely accepted as essential to reduce the risk of infection following CD. Current guidelines recommend an intravenous (IV) first-generation cephalosporin 30-60 minutes before the caesarean incision, being cefazolin the most used [9,11]. However, given the persistent occurrence of infections, the current standard antibiotic prophylaxis appears to be insufficient. Ureaplasma spp. and Mycoplasma spp. are considered major pathogens in the development of endometritis and wound infection. As they do not take part in the cefazolin action spectrum, some authors propose using azithromycin, a broad-spectrum macrolide, as an extended-spectrum prophylactic agent, given its efficacy against these microorganisms [11,12].
Therefore, our aim is to identify scientific evidence on whether broadening the antimicrobial spectrum by combining azithromycin with a first-generation cephalosporin can reduce the incidence of post-caesarean delivery infections, without causing any adverse or undesirable effects on both mother and neonate.
Methodology
For this narrative review, a bibliographic search was conducted using the following Medical Subject Headings (MeSH): “Azithromycin”, “Caesarean Section”, “Caesarean Section/ adverse effects”, “Elective Caesarean Delivery”, “Non elective Caesarean Delivery”, “Endometritis/ prevention & control” and “Surgical Wound Infections/ prevention & control”. The search was carried out in several databases, including Embase, Google Scholar, Medline, PubMed and Scopus. Additional relevant publications were identified by screening the reference lists of the selected articles. The WHO’s recommendations relating to CD were consulted.
The inclusion criteria comprised clinical trials, systematic reviews, meta-analyses and observational studies (cohort, case-control, and cross-sectional) related to the topic and published in Portuguese or English, between 1985 and May 2025. Articles focusing on the treatment of SSIs rather than their prevention, as well as those for which the full text was not available, were excluded. A total of 61 articles were selected.
Indications for Caesarean Delivery
CD is a life-saving obstetric surgical procedure performed as an alternative to a vaginal birth. Cesarean deliveries have undergone multiple transformations to become a safer procedure. However, postoperative complications, particularly post-caesarean infections and hemorrhage, continue to occur. The rising rates of CDs in recent decades deserve careful consideration, as they are associated with more complications. Therefore, a CD should only be performed when there is clear medical evidence supporting its benefits [3,13-15].
According to timing, CDs can be classified into two groups: elective, which is planned for medical reasons before labor begins; and nonelective, which is performed after labor begins, without prior planning [14,16,17[. Nonelective CDs are more common than elective ones, with respective rates of 78% and 22% [17]. There is no consensus regarding significant differences in the incidence of infections between elective and non-elective CDs [16,18,19].
Indications for Elective Caesarean Delivery
The most common reason for an elective CD is fetus malpresentation [7,17]. Other reasons include previous caesarean section. In twin pregnancies, delivery should be performed by caesarean section if the first twin is not in cephalic presentation or in case of a monochorionic monoamniotic pregnancy [20]. CD is also recommended in triplet pregnancy [7,21]. Placenta previa is another indication, in which the placenta partially or completely covers the cervical os, and vasa previa, where the fetal blood vessels run between the fetus and the cervical os.
Planned CD for isolated macrosomia only if the fetus is estimated to weigh more than 5000 g in non-diabetic mothers or more than 4500 g in diabetic mothers [21].
Additional situations that should be considered include fetal growth restriction, maternal obesity, and active genital herpes, these should be evaluated on a case-by-case basis. According to current guidelines, a maternal request for a CD based on anxiety related to childbirth or fear of labor pain is not regarded as a valid indication for CD [14,16,20].
Indications for Nonelective Caesarean Delivery
One of the main indications for nonelective caesarean sections is dystocia, which is failure to progress in labor and signs of fetal distress, such as hypoxia, acidosis or cord prolapse, which compromise fetal blood flow. In the presence of dystocia, the underlying causes may include: absolute cephalopelvic disproportion, fetal malposition or inadequate uterine contractions [21].
Although it does not occur after the onset of labor, there is an emergency obstetric condition that may be included among the indications for nonelective CD. This condition, known as abruptio placentae, refers to the premature separation of a normally implanted placenta from the uterine wall, leading to severe hemorrhage [22].
Intraoperative Workflow for Caesarean Delivery
The perioperative CD pathway begins with the administration of antibiotic prophylaxis 30 to 60 minutes before the skin incision. Current guidelines recommend the use of a first-generation cephalosporin, the cefazolin, 1-2 g IV [9,23].
Patient preparation should begin with a full-body bath24. The surgical site skin must be disinfected with an alcohol-based antiseptic solutions containing chlorhexidine gluconate, to remove the endogenous flora [25]. Vaginal preparation consists in antiseptic cleansing with povidone-iodine solution [26]. Surgical field sterility must be ensured prior to incision [26,27].
The subsequent step involves neuraxial anesthesia, which improves postoperative recovery and reduces the incidence of SSI compared to general anesthesia [28]. Caesarean sections begin with a scalpel transverse suprapubic incision in the skin [29]. The scalpel first incises the skin, then proceeds through the subcutaneous tissue and the fascial layer, before finally reaching the parietal peritoneum [30].
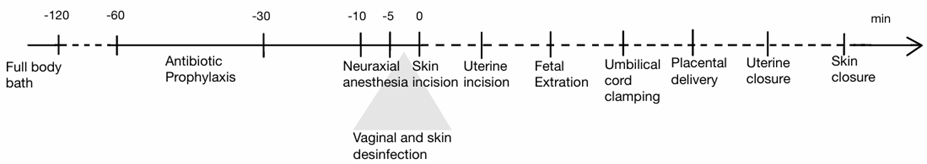
The uterine incision with approximately 3 cm, is typically made transversely in the lower segment of the uterus and extended bluntly with two indexes of the surgeon’s fingers [31]. Once the uterine incision reaches approximately 10 cm, the fetal extraction should be performed in an atraumatic manner. Once the newborn has established spontaneous respiration, the umbilical cord should be clamped, usually delayed for at least one minute [26]. The placenta is expelled spontaneously with gentle cord traction and uterine massage. Removing it through cord traction reduces the risk of post-caesarean endometritis [32]. Uterine closure is then performed, commonly using a double- layer technique with a continuous unlocked suture [26]. This is followed by closure of the rectus muscle fascia, subcutaneous tissue and, finally, the skin. Skin closure can be performed using either non-absorbable staples or absorbable subcutaneous sutures, with similar rates of wound infection [29] (Figure 1).
Figure 1: Intraoperative workflow for caesarean delivery, with a particular emphasis on the key moments for infection prophylaxis. The dotted line in the timeline represents a nonspecific time interval, dependent on the surgical procedure and its intraoperative course [24,26,29,30,33].
Caesarean Delivery Complications
Caesarean births can result in both short and long-term complications [4]. Long-term risks regarding future pregnancies include placenta previa, placenta accreta, caesarean scar pregnancy and uterine rupture. Gynecological complications may involve chronic abdominal pain, pelvic adhesions, infertility and irregular bleeding [2]. In the short-term complications, intraoperative risks are hemorrhage, extension of the uterine incision and bladder injury. Postoperative complications include endometritis, wound infection, urinary tract infection, spinal headache, disseminated intravascular coagulation, maternal sepsis, and maternal death [6]. As a surgical procedure, it is associated with risks such as adverse reactions to anesthesia, blood vessels damage or injury to other organs [16].
Post-Caesarean Infections
A wide range of postoperative infections may occur following a CD. According to the WHO, the most common are SSI, with a rate of 20% in Africa vs 2,9% in Europe [11,25,34]. As expected, lower income countries are associated with higher rates of infectious complications [8]. The US Centers for Disease Control and Prevention classify SSI into three groups: superficial incision, deep incision and organ incision. This classification is based on the time after surgery, the anatomical location involved, the presence of clinical signs or symptoms and microbiological tests. Any other possible causes of these symptoms should be excluded (Table 1) [11,35,36].
Table 1: Classification and diagnosis of SSI, as defined by the Centers for Disease Control and Prevention. Based on CDC, Ncezid, DHQP. Surgical Site Infection Event (SSI) [Internet]. Based on: https://www.cdc.gov/nhsn/pdfs/ps-analysis-resources/ImportingProcedureData.pdf
| Superficial SSI | Deep SSI | Organ SSI | |
| Timing | 30 days after surgical procedure | 30-90 days after surgical procedure | 30-90 days after surgical procedure |
| Local | Skin Subcutaneous tissue | Fascia Muscle layers | Uterus |
| Criteria | a. Purulent drainage. | a. Purulent drainage. | a. Organisms identified from endometrial fluid by a microbiological test. |
| b. Microorganisms identified in superficial incision/subcutaneous tissue by a microbiologic analysis, after it is opened by a surgeon. | b. Microorganisms identified by a microbiologic test in patients with fever less than 38°C) or localized pain or presence of an abscess, after it is opened by a surgeon. | b. Suspect of endometritis with at least two of the following symptoms: fever (>38°C), uterine/abdominal pain or tenderness, purulent drainage from the uterus AND exclusion of other possible causes. | |
| c. Typical inflammation signs as localized pain or tenderness, swelling, edema, erythema and heat. | c. An abscess or other infection involving deep tissues, detected by complementary medical exams. | ||
| d. Superficial incision SSI diagnoses by a doctor. | |||
| Diagnosis | 1 of the previous criteria | ||
| Classification | Wound Infection | Endometritis | |
The WHO defines maternal sepsis as a “life-threatening condition that arises when the body’s response to infection causes injury to its own tissues and organs during pregnancy, childbirth, post-abortion or the postpartum period”. It is the most feared complication of CD and remains the third most common cause of maternal mortality, accounting for 11% of maternal deaths [37,38]. Failure to treat or manage the afore mentioned infections appropriately may lead to the progression of the infection to sepsis [11].
Microorganisms Involved in Post-Caesarean Delivery Infections
The mechanism of postpartum endometritis is analogous to that of a surgical wound infection. It results from the contamination of the uterine cavity and skin with lower vaginal tract macrobian flora and endogenous skin flora [27,39].
Gardnerella vaginalis is responsible for the disruption of the normal vaginal flora, a condition known as bacterial vaginosis. Its presence increases the risk of uterine contamination during CD, increasing the risk of post-caesarean endometritis in six times. Treating bacterial vaginosis during pregnancy reduces the rate of endometritis rates after CD, antimicrobial options include metronidazole or clindamycin, orally or intravaginally [19,40,41].
Post-caesarean infections are predominantly polymicrobial. Endometritis is mainly caused by a combination of aerobic and anaerobic bacteria. Examples of aerobes include Streptococcus spp., Staphylococcus aureus, Escherichia coli, Klebsiella pneumoniae, Enterococcus faecalis, Proteus mirabilis, Ureaplasma urealyticum, and Mycoplasma hominis. Anaerobes include Bacteroides spp., Clostridium spp., Peptostreptococcus spp., Peptococcus spp., and Prevotella spp [12,19,39,42-44]. The most common pathogens isolated from post-CD wound infections are Ureaplasma urealyticum, Mycoplasma hominis, as well as Escherichia coli, Streptococcus spp., Staphylococcus aureus, Klebsiella pneumoniae, Proteus mirabilis, and Enterococcus faecalis (Table 2) [27,45-47].
Table 2: Microorganisms causing post-caesarean delivery wound infection and endometritis [27,39,46,47].
| Endometritis | Wound Infection |
| Ureaplasma urealyticum | |
| Mycoplasma hominis | |
| Escherichia Coli | |
| Streptococcus spp. | |
| Staphylococcus aureus | |
| Klebsiella pneumoniae | |
| Proteus mirabilis | |
| Enterococcus faecalis | |
| Gardnerella vaginalis | |
| Bacteroides spp. | |
| Fusobacterium spp. | |
| Clostridium spp. | |
| Peptostreptococcus spp. | |
| Peptococcus spp. | |
| Prevotella spp. | |
Prophylactic Antibiotic Therapy in Caesarean Delivery
The purpose of antibiotic prophylaxis is to prevent, rather than to treat established infections. Therefore, prophylactic antibiotics must be administered before potential bacterial contamination occurs to ensure adequate tissue concentrations at the time of microbial exposure [23]. The main risk associated with antibiotic prophylaxis is the development of antimicrobial resistance [48].
According to the WHO, routine antibiotic prophylaxis is recommended for women undergoing elective or non-elective caesarean delivery. When performing a CD, a single IV dose of first- generation cephalosporins should be administered 30 to 60 minutes before skin incision [9].
First-generation cephalosporins have been chosen based on their mechanism of action, broad spectrum of activity, and global availability [9,49]. Their main mechanism of action involves disrupting the construction of the bacterial cell wall, by causing the rupture of the cross-linking between peptidoglycan chains [50]. They are effective against gram-positive aerobic bacteria, such as Staphylococcus aureus, Staphylococcus epidermidis, Streptococcus pyogenes, Streptococcus agalactiae, Streptococcus pneumonia and Streptococcus bovis. They also exhibit modest activity against Escherichia coli, Moraxella catarrhalis, Klebsiella pneumoniae, and Proteus mirabilis [49,51]. However, this prophylaxis fails to provide coverage against Ureaplasma spp. and Mycoplasma spp., as these organisms lack a peptidoglycan cell wall that is the main target of cephalosporins [50]. Both Ureaplasma spp. and Mycoplasma spp. are mainly involved in post-CD infections [12,45[.
The current prophylactic antibiotic regimen for CD typically consists of 1-2 g of IV cefazolin, with the dose adjusted according to maternal weight: 1g for women weighing less than 80 kg, and 2 g for those weighing more than 80 kg [23]. Evidence suggests that broadening the antibiotic spectrum can reduce the risk of surgical site infection and the incidence of endometritis by 25% [11]. That is why several authors have proposed adding azithromycin as an adjunct [11,52,53].
Azithromycin
Azithromycin is a second-generation macrolide antibiotic with a broad spectrum of activity. It is particularly effective against Ureaplasma spp., and Mycoplasma spp., which are among the most frequently isolated pathogens in post-caesarean delivery infections [45]. Its mechanism of action involves inhibition of bacterial protein synthesis through binding to the 50S ribosomal subunit. It achieves high concentrations at infection sites due to its accumulation in phagocytes that migrate to these areas [54,55]. Azithromycin is indicated for respiratory, urogenital, dermal, and other bacterial infections, due to its broad-spectrum activity, including Ureaplasma spp., Mycoplasma spp., Chlamydia trachomatis, Neisseria gonorrhoea and Streptococcus spp. It has been described as a safe and well-tolerated antibiotic [54].
A single 500 mg dose of azithromycin administered prior to skin incision achieves adequate plasma and myometrial concentrations for prophylaxis against Ureaplasma spp. [53]. A single 500 mg dose of azithromycin provides a prolonged serum half-life of approximately 50 hours, which is advantageous for prophylactic use given that the highest risk period for postoperative infection is within the first 48 hours after skin incision [55]. It is generally well tolerated and has a favorable safety profile. However, there are concerns about its potential cardiac effects, particularly the possible risk of QT interval prolongation, which has only been reported in a few cases [54].
To make the antibiotic spectrum and its role in the prophylaxis for post-caesarean infections easier to understand, we created a Venn diagram showing both the spectrum of cefazolin and azithromycin, as well as the microorganisms most involved in post-CD infections (Figure 2).
Figure 2: Venn diagram illustrating the microorganisms involved in post-caesarean infections and the antibiotic spectrum of action [12,27,39,49-51,54].
Although concerns are often raised about the potential development of antimicrobial resistance when the spectrum of prophylactic antibiotics is broadened, this is highly improbable, as a single administration does not contribute to the emergence of resistance [42,56].
Azithromycin Plus Cefazolin Prophylaxis for Caesarean Delivery
Tita et al. (2016) conducted a study comparing the prophylactic administration of cefazolin (1-2 g IV) plus azithromycin (500 mg in 250 ml of saline, IV) with cefazolin (1-2 g IV) plus a placebo in women undergoing nonelective CD. The study demonstrated that the addition of azithromycin to cefazolin significantly reduced the risk of endometritis (from 6.1% to 3.8%), wound infection (from 6.6% to 2.4%), and serious maternal adverse events (from 2.9% to 1.5%). There was no significant difference in the incidence of other infectious complications, such as abdominal or pelvic abscess, septic pelvic thrombophlebitis, maternal sepsis, pyelonephritis, meningitis and pneumonia between the two groups. The study demonstrated that extending the prophylactic antibiotic spectrum with azithromycin significantly decreased the incidence of postpartum infections without any adverse effects on newborns. This trial included only women undergoing nonelective CD, which is a limitation [11].
Jyothi M. et al. (2019) conducted a randomized controlled trial to evaluate the efficacy of cefazolin plus azithromycin for antibiotic prophylaxis in CD, including both elective and nonelective procedures. Participants were allocated into two groups: one received prophylactic cefazolin (2 g IV) plus a placebo, and the other group received cefazolin (2 g IV) plus azithromycin (500 mg IV). The study demonstrated a significant reduction in the incidence of surgical site infection in the azithromycin group (from 15% to 3%), as well as a lower rate of endometritis (from 10% to 2%)19. Pierce et al. (2021) conducted a retrospective cohort study from 2016 to 2018, including women who underwent elective and nonelective CD. The first group from march 2016 to october 2017 received cefazolin (2g IV) and the second between september and august 2018 received cefazolin (2g IV) plus 500 mg of IV azithromycin. Unlike other studies, the addiction of azithromycin did not show a statistically significant difference in the incidence of post-caesarean infections between groups [57].
Ruzic et al. (2023) conducted a retrospective cohort study from 2013 to 2018. The study included women who underwent elective CD for a singleton neonate. The participants were divided into two groups. The first from january 2013 to october 2015, these patients received cefazolin (2g IV if < 120>120 kg). The second group comprised women who gave birth between january 2016 and december 2018 with the same cefazolin regimen, plus a 500 mg IV of azithromycin. A significantly lower incidence of composite post-caesarean infections was demonstrated (falling from 4.8% to 3.3%), primarily due to a marked reduction in wound infections (falling from 3.9% to 2.4%) among patients who received combined pre-labor prophylaxis. There were no significant differences in the incidence of endometritis, intra-abdominal abscess or urinary tract infections between the two groups [52].
Regarding economic considerations, Skeith A et al. (2017) conducted a study which demonstrated that the use of adjunctive azithromycin alongside cefazolin is more cost-effective than cefazolin alone. Since it avoids hospitalizations and treatments, which are associated with healthcare costs [58].
Few studies have addressed this specific topic. Based on the available literature, three out of four studies have demonstrated that using prophylactic cefazolin combined with azithromycin reduces the incidence of post-caesarean infections in CD, with a reduction in wound infections being the most consistently reported outcome. Additionally, this combined regimen has been shown to offer cost-effectiveness advantages [11,59,60]. However, one study found no significant differences between groups receiving cefazolin alone or in combination with azithromycin [57]. While the current evidence suggests that azithromycin shows promising results, further research is needed. Future studies should include large-scale randomized controlled trials to confirm these findings, assess long-term maternal and neonatal outcomes, and evaluate potential antimicrobial resistance patterns associated with broader antibiotic use.
Conclusion
Post-CD infections remain a major clinical concern. Despite significant medical advances in recent years, such as aseptic techniques and antibiotic prophylaxis, the incidence of post- caesarean infections remains higher than desired, contributing to considerable maternal morbidity. Current evidence indicates that cefazolin alone may be an insufficient prophylactic agent, as it does not cover some bacteria, such as Mycoplasma spp. and Ureaplasma spp., which are implicated in many post-caesarean infections, including wound infections and endometritis. This scientific evidence supports the need to broaden the antimicrobial spectrum.
Azithromycin is a broad-spectrum macrolide that is highly effective against the microorganisms mentioned previously. Moreover, several studies have demonstrated a significant reduction in infectious morbidity following caesarean when azithromycin is used as an adjunct to cefazolin. However, not all studies addressing this issue have reported consistent findings, one study observed no significant difference in infectious outcomes with the addition of azithromycin to prophylactic procedures.
A randomized controlled trial called the “Azithromycin Prophylaxis for Prelabor Cesarean Delivery Trial” is currently evaluating the administration of azithromycin in combination with cefazolin in CD. The findings of this study will be highly relevant to the conclusions on this matter [61].
Based on the currently available scientific evidence, we conclude that adding 500 mg of IV azithromycin to the standard antibiotic prophylaxis regimen for CD may be beneficial in reducing infectious morbidity following the procedure. Alongside antibiotic prophylaxis, other strategies should be implemented to reduce the incidence of post-caesarean complications, particularly by minimizing the number of unnecessary caesarean deliveries. Furthermore, optimizing perioperative practices, such as proper skin antisepsis, weight-adjusted antibiotic dosing and adherence to aseptic surgical techniques may further decrease postoperative infection rates. Future research should aim to confirm these findings through large-scale randomized trials, as well as evaluating the long-term safety of azithromycin, particularly regarding antimicrobial resistance and its potential impact on the maternal and neonatal microbiome.
Abbreviations and Acronym List
CD: Caesarean Delivery
IV: Intravenous
MeSH: Medical Subject Headings
SSI: Surgical Site Infection
WHO: World Health Organization
References
- World Health Organization. (2018). WHO Recommendations Non-Clinical Interventions to Reduce Unnecessary Caesarean Sections. World Health Organization.
Publisher | Google Scholor - Antoine, C., Young, B. K. (2021). Cesarean Section One Hundred Years 1920-2020: The Good, The Bad and The Ugly. Journal of Perinatal Medicine, 49(1):5-16.
Publisher | Google Scholor - Sparić, R., Kadija, S., Hudelist, G., Glišić, A., Buzadžić, S. (2012). History of Caesarean Hysterectomy. Acta Chirurgica Iugoslavica, 59(1): 9-12.
Publisher | Google Scholor - Sandall, J., Tribe, R. M., Avery, L., Mola, G., Visser, G. H., et al. (2018). Short-Term and Long-Term Effects of Caesarean Section on The Health of Women and Children. The Lancet, 392(10155):1349-1357.
Publisher | Google Scholor - World Health Organization. (2025). Robson Classification Platform.
Publisher | Google Scholor - Agrawal, S., Agarwal, V. K. (2018). Maternal and Fetal Outcome in Emergency Versus Elective Caesarean Section. Int J Reprod Contracept Obstet Gynecol, 7(12):4845.
Publisher | Google Scholor - Gregory, K. D., Korst, L. M., Gornbein, J. A., Platt, L. D. (2002). Using Administrative Data to Identify Indications for Elective Primary Cesarean Delivery. Health Services Research, 37(5):1387-1401.
Publisher | Google Scholor - Bonet, M., Brizuela, V., Abalos, E., Cuesta, C., Baguiya, A., et al. (2020). Frequency and Management of Maternal Infection in Health Facilities in 52 Countries (GLOSS): A 1-Week Inception Cohort Study. The Lancet Global Health, 8(5):e661-e671.
Publisher | Google Scholor - World Health Organization. (2021). Prophylactic Antibiotics for Women Undergoing Caesarean Section.
Publisher | Google Scholor - Chelmow, D., Ruehli, M. S., Huang, E. (2001). Prophylactic Use of Antibiotics for Nonlaboring Patients Undergoing Cesarean Delivery with Intact Membranes: A Meta-Analysis. American Journal of Obstetrics and Gynecology, 184(4):656-661.
Publisher | Google Scholor - Tita, A. T., Szychowski, J. M., Boggess, K., Saade, G., Longo, S., et al. (2016). Adjunctive Azithromycin Prophylaxis for Cesarean Delivery. New England Journal of Medicine, 375(13):1231-1241.
Publisher | Google Scholor - Andrews, W. W., Shah, S. R., Goldenberg, R. L., Cliver, S. P., Hauth, J. C., et al. (1995). Association of Post-Cesarean Delivery Endometritis with Colonization of The Chorioamnion by Ureaplasma Urealyticum. Obstetrics & Gynecology, 85(4):509-514.
Publisher | Google Scholor - Betrán, A. P., Ye, J., Moller, A. B., Zhang, J., Gülmezoglu, A. M., et al. (2016). The Increasing Trend in Caesarean Section Rates: Global, Regional and National Estimates: 1990-2014. PloS one, 11(2):e0148343.
Publisher | Google Scholor - Stjernholm, Y. V., Petersson, K., Eneroth, E. (2010). Changed Indications for Cesarean Sections. Acta Obstetricia et Gynecologica Scandinavica, 89(1):49-53.
Publisher | Google Scholor - Mylonas, I., Friese, K. (2015). Indications for and Risks of Elective Cesarean Section. Deutsches Ärzteblatt International, 112(29-30):489.
Publisher | Google Scholor - Wagner, M. (2000). Choosing Caesarean Section. The Lancet, 356(9242):1677-1680.
Publisher | Google Scholor - Naeem, M., Khan, M. Z. U. I., Abbas, S. H., Khan, A., Adil, M., et al. (2015). Rate and Indications of Elective and Emergency Caesarean Section; A Study in a Tertiary Care Hospital of Peshawar. Journal of Ayub Medical College Abbottabad, 27(1):151-54.
Publisher | Google Scholor - Kristian Opøien, H., Valbø, A., Grinde-Andersen, A., Walberg, M. (2007). Post-Cesarean Surgical Site Infections According to CDC Standards: Rates and Risk Factors. A Prospective Cohort Study. Acta Obstetricia et Gynecologica SCANDINAVICA, 86(9):1097-1102.
Publisher | Google Scholor - Jyothi, M. S., Kalra, J. K., Arora, A., Patil, A., Suri, V., et al. (2019). Randomized Controlled Trial of Cefazolin Monotherapy Versus Cefazolin Plus Azithromycin Single Dose Prophylaxis for Cesarean Deliveries: A Developing Country's Perspective. Journal of Family Medicine and Primary Care, 8(9):3015-3021.
Publisher | Google Scholor - Coates, D., Homer, C., Wilson, A., Deady, L., Mason, E., et al. (2020). Indications for, and Timing of, Planned Caesarean Section: A Systematic Analysis of Clinical Guidelines. Women and Birth, 33(1):22-34.
Publisher | Google Scholor - Penn, Z., Ghaem-Maghami, S. (2001). Indications for Caesarean Section. Best Practice & Research Clinical Obstetrics & Gynaecology, 15(1):1-15.
Publisher | Google Scholor - Musarrat J, Fouzia G. (2004). Abruptio Placentae: Risk Factors and Perinatal Outcome. JPMI, 18:6696.
Publisher | Google Scholor - The American College of Obstetricians and Gynecologists. (2011). ACOG PRACTICE BULLETIN Clinical Management Guidelines for Obstetrician-Gynecologists.
Publisher | Google Scholor - Tanner, J., Melen, K. (2021). Preoperative Hair Removal to Reduce Surgical Site Infection. Cochrane Database of Systematic Reviews, (8).
Publisher | Google Scholor - World Health Organization. (2018). Protocol for Surgical Site Infection Surveillance with a Focus on Settings with Limited Resources.
Publisher | Google Scholor - Caughey, A. B., Wood, S. L., Macones, G. A., Wrench, I. J., Huang, J., et al. (2018). Guidelines for Intraoperative Care in Cesarean Delivery: Enhanced Recovery After Surgery Society Recommendations (Part 2). American Journal of Obstetrics and Gynecology, 219(6):533-544.
Publisher | Google Scholor - Owen, J., Andrews, W. W. (1994). Wound Complications after Cesarean Sections. Clinical Obstetrics and Gynecology, 37(4):842-855.
Publisher | Google Scholor - Watson, S. E., Richardson, A. L., Lucas, D. N. (2022). Neuraxial and General Anaesthesia for Caesarean Section. Best Practice & Research Clinical Anaesthesiology, 36(1):53-68.
Publisher | Google Scholor - Mackeen, A. D., Berghella, V., Larsen, M. L. (2012). Techniques and Materials for Skin Closure in Caesarean Section. Cochrane Database of Systematic Reviews, (9).
Publisher | Google Scholor - Dodd, J. M., Anderson, E. R., Gates, S., Grivell, R. M. (2014). Surgical Techniques for Uterine Incision and Uterine Closure at The Time of Caesarean Section. Cochrane Database of Systematic Reviews, (7).
Publisher | Google Scholor - Vikhareva O, Rickle GS, Lavesson T, Nedopekina E, Brandell K, et al. (2019). Hysterotomy Level at Cesarean Section and Occurrence of Large Scar Defects: A Randomized Single-Blind Trial. Ultrasound Obstet Gynecol. 53(4):438-442.
Publisher | Google Scholor - Anorlu, R. I., Maholwana, B., Hofmeyr, G. J. (2008). Methods of Delivering the Placenta at Caesarean Section. Cochrane Database of Systematic Reviews, (3).
Publisher | Google Scholor - Dahlke, J. D., Mendez-Figueroa, H., Rouse, D. J., Berghella, V., Baxter, J. K., et al. (2013). Evidence-Based Surgery for Cesarean Delivery: An Updated Systematic Review. American Journal of Obstetrics and Gynecology, 209(4):294-306.
Publisher | Google Scholor - World Health Organization. (2016). Global guidelines for the prevention of surgical site infection. World Health Organization.
Publisher | Google Scholor - CDC, Ncezid, DHQP. Surgical Site Infection (SSI) Event.
Publisher | Google Scholor - CDC, Ncezid, DHQP. CDC/NHSN Surveillance Definitions for Specific Types of Infections.
Publisher | Google Scholor - Bonet, M., Souza, J. P., Abalos, E., Fawole, B., Knight, M., et al. (2018). The Global Maternal Sepsis Study and Awareness Campaign (GLOSS): Study Protocol. Reproductive Health, 15(1):16.
Publisher | Google Scholor - World Health Organization. (2015). WHO recommendations for prevention and treatment of maternal peripartum infections. World Health Organization.
Publisher | Google Scholor - Sherman, D., Lurie, S., Betzer, M., Pinhasi, Y., Arieli, S., et al. (1999). Uterine Flora at Cesarean and Its Relationship to Postpartum Endometritis. Obstetrics & Gynecology, 94(5):787-791.
Publisher | Google Scholor - Newton, E. R., Wallace, P. A. (1998). Effects of Prophylactic Antibiotics on Endometrial Flora in Women with Postcesarean Endometritis. Obstetrics & Gynecology, 92(2):262-268.
Publisher | Google Scholor - Ziogou, A., Ziogos, E., Giannakodimos, I., Giannakodimos, A., Sifakis, S., et al. (2023, April). Bacterial vaginosis and post-operative pelvic infections. In Healthcare, 11(9):1218.
Publisher | Google Scholor - Singh, N., Sethi, A. (2022). Endometritis-Diagnosis, Treatment and Its Impact on Fertility-A Scoping Review. JBRA Assisted Reproduction, 26(3):538.
Publisher | Google Scholor - de Oliveira Ferreira, D., de Macêdo Costa, M. G., dos Santos Belarmino, R., Morais, D. B., Mota, K. B., et al. (2025). Defining a Panel of Principal Bacteria Associated with Endometritis. JBRA Assisted Reproduction, 29(1):150.
Publisher | Google Scholor - Rosene, K., Eschenbach, D. A., Tompkins, L. S., Kenny, G. E., Watkins, H. (1986). Polymicrobial Early Postpartum Endometritis with Facultative and Anaerobic Bacteria, Genital Mycoplasmas, and Chlamydia Trachomatis: Treatment with Piperacillin or Cefoxitin. Journal of Infectious Diseases, 153(6):1028-1037.
Publisher | Google Scholor - Tita, A. T., Rouse, D. J., Blackwell, S., Saade, G. R., Spong, C. Y., et al. (2009). Emerging Concepts in Antibiotic Prophylaxis for Cesarean Delivery: A Systematic Review. Obstetrics & Gynecology, 113(3):675-682.
Publisher | Google Scholor - Zuarez-Easton, S., Zafran, N., Garmi, G., Salim, R. (2017). Postcesarean Wound Infection: Prevalence, Impact, Prevention, and Management Challenges. International Journal of Women's Health, 9:81-88.
Publisher | Google Scholor - Kawakita, T., Landy, H. J. (2017). Surgical Site Infections After Cesarean Delivery: Epidemiology, Prevention and Treatment. Maternal Health, Neonatology and Perinatology, 3(1):12.
Publisher | Google Scholor - The American College of Obstetricians and Gynecologists. (2011). ACOG PRACTICE BULLETIN Clinical Management Guidelines for Obstetrician-Gynecologists.
Publisher | Google Scholor - Pacifici, G. M. (2022). Clinical Pharmacology of Cefazolin. Advances in Biomedical and Health Sciences, 1(4):196-202.
Publisher | Google Scholor - Lin, X., Kück, U. (2022). Cephalosporins as Key Lead Generation Beta-Lactam Antibiotics. Applied Microbiology and Biotechnology, 106(24):8007-8020.
Publisher | Google Scholor - Zhang, S. X., Parisian, F., Yau, Y., Fuller, J. D., Poutanen, S. M., et al. (2007). Narrow-Spectrum Cephalosporin Susceptibility Testing of Escherichia Coli with The BD Phoenix Automated System: Questionable Utility of Cephalothin as a Predictor of Cephalexin Susceptibility. Journal of Clinical Microbiology, 45(11):3762-3763.
Publisher | Google Scholor - Ruzic, M. F., Blanchard, C. T., Cozzi, G. D., Howard, H. R., Casey, B. M., et al. (2023). Adjunctive Azithromycin Prophylaxis for Prelabor Cesarean Birth. Obstetrics & Gynecology, 141(2):403-413.
Publisher | Google Scholor - Sutton, A. L., Acosta, E. P., Larson, K. B., Kerstner-Wood, C. D., Tita, A. T., et al. (2015). Perinatal Pharmacokinetics of Azithromycin for Cesarean Prophylaxis. American Journal of Obstetrics and Gynecology, 212(6):812-e1.
Publisher | Google Scholor - Parnham, M. J., Haber, V. E., Giamarellos-Bourboulis, E. J., Perletti, G., Verleden, G. M., et al. (2014). Azithromycin: Mechanisms of Action and Their Relevance for Clinical Applications. Pharmacology & Therapeutics, 143(2):225-245.
Publisher | Google Scholor - Heidary, M., Ebrahimi Samangani, A., Kargari, A., Kiani Nejad, A., Yashmi, I., et al. (2022). Mechanism of action, resistance, synergism, and clinical implications of azithromycin. Journal of Clinical Laboratory Analysis, 36(6):e24427.
Publisher | Google Scholor - Ahmed, N. J., Haseeb, A., AlQarni, A., AlGethamy, M., Mahrous, A. J., et al. (2023). Antibiotics for Preventing Infection at The Surgical Site: Single Dose Vs. Multiple Doses. Saudi Pharmaceutical Journal, 31(12):101800.
Publisher | Google Scholor - Pierce, S. L., Bisson, C. M., Dubois, M. E., Grimes, S. B., Katz, M. S., et al. (2021). Clinical effectiveness of adding azithromycin to antimicrobial prophylaxis for cesarean delivery. American Journal of Obstetrics and Gynecology, 225(3):335-e1.
Publisher | Google Scholor - Skeith, A. E., Niu, B., Valent, A. M., Tuuli, M. G., Caughey, A. B. (2017). Adding azithromycin to cephalosporin for cesarean delivery infection prophylaxis: a cost-effectiveness analysis. Obstetrics & Gynecology, 130(6):1279-1284.
Publisher | Google Scholor - Tita, A. T., Owen, J., Stamm, A. M., Grimes, A., Hauth, J. C., et al. (2008). Impact of Extended-Spectrum Antibiotic Prophylaxis on Incidence of Postcesarean Surgical Wound Infection. American Journal of Obstetrics and Gynecology, 199(3):303-e1.
Publisher | Google Scholor - Ward, E., Duff, P. (2016). A Comparison of 3 Antibiotic Regimens for Prevention of Postcesarean Endometritis: An Historical Cohort Study. American Journal of Obstetrics and Gynecology, 214(6):751-e1.
Publisher | Google Scholor - Azithromycin Prophylaxis for Prelabor Cesarean Delivery Trial (PRECEDE). ClinicalTrials.gov.
Publisher | Google Scholor