Research Article
Puncture Laser Microdiscectomy in Elderly Patients with Protrusions and Hernias of The Lumbar Spine
- Zorin M.O *
Department of Nervous Diseases and Neurosurgery, Faculty of Postgraduate Education, Dnipro State Medical University, Dnipro, MC "Endoscopic Neurosurgery", Dnipro, Ukraine.
*Corresponding Author: Zorin M.O,Department of Nervous Diseases and Neurosurgery, Faculty of Postgraduate Education, Dnipro State Medical University, Dnipro, MC
Citation: Zorin M.O. (2026). Puncture Laser Microdiscectomy in Elderly Patients with Protrusions and Hernias of The Lumbar Spine. Journal of Neuroscience and Neurological Research. BioRes Scientia Publishers. 5(1):1-4. DOI: 10.59657/2837-4843.brs.26.034
Copyright: © 2026 Zorin M.O, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: May 15, 2025 | Accepted: January 15, 2026 | Published: January 22, 2026
Abstract
Objective: To improve the results of puncture laser microdiscectomy in elderly patients with protrusions and hernias of the lumbar spine.
Materials and methods; The work was performed at the Endoscopic Neurosurgery Medical Center in Dnipro, Ukraine. The study included 530 patients aged 50 to 72 years, with an average age of 58.6±5.63 years. There were 260 men and 270 women. Of all 530 patients, 2 groups were formed: in group I there were patients who underwent PLMD of one or, if necessary, two MHDs, with the presence of protrusions (410), in group II PLMD was performed MHD with hernia (120 patients). The examined group included patients whose age exceeded 50 years, the affected discs retained hydrophilicity and sufficient disc height (not less than 2/3 of the norm), the sagittal size of the hernia did not exceed 6 mm, there was no ossifying ligamentosis, no degenerative stenosis of the spinal canal, and no spondylolisthesis. Protrusions of 3 to 5 mm in size were taken into account. Pain was assessed before surgery and within 2 weeks using the VAS scale. The effectiveness of surgery after one month was assessed using the McNab scale.
Results. In elderly patients, pain increases slightly during the first week after PLMD, which is explained by the aseptic inflammatory reaction of the tissues surrounding the MCD. By the end of the month, the inflammatory reaction regresses, but the pain still remains at a high level. In our opinion, this is associated with less elasticity and a lower tendency to repair in elderly patients. But after 3 months, the condition of such patients improved significantly, as evidenced by the results of our examination with assessment on the McNab scale.
Conclusions: Temporary deterioration of the condition of elderly patients within a month after PLMD is explained by aseptic inflammation of the tissues surrounding the MCD and a decrease in elasticity and a decrease in the tendency to repair in such patients. With the correct selection of elderly patients, PLMD can be quite effective.
Keywords: puncture laser microdiscectomy; protrusions and hernias of the lumbar spine; advanced age
Introduction
According to many scientific studies, in young and middle-aged patients, both radicular pain and low back pain are significantly reduced one month after PLMD. Of course, degenerative spinal disorders (DSD) are primarily a disease of the elderly. At the same time, the majority of medical technologies concern patients of middle and working age. This also applies to puncture lumbar microdiscectomy (PLMD), which has confidently entered clinical practice since the 1980s and to this day occupies a significant place in the treatment of DSD [1,2]. This technique is called differently: nucleoplasty, intradiscal decompression, vaporization, etc. [3,4,5] At the suggestion of E.G. Pedachenko, this method is called “puncture laser microdiscectomy” [6]. We support this name because experimental and clinical studies have shown that, as a result of the ablation and vaporization effect, the laser beam significantly reduces the volume of the intervertebral disc (IDC) by 15-25% [7]. Despite the fact that most ICD protrusions are asymptomatic, there are protrusions that cause not only local pain syndrome in the lower back (lumbalgia), but also, not infrequently, radicular pain syndrome. As for hernias of lumbar MCD, they are more characterized by radicular pain syndrome and, to a lesser extent, lumbalgia. It is known that most protrusions are successfully treated with conservative methods. The same applies to hernias of small size, up to 6 mm without signs of sequestration [8]. But a relatively small group of such patients do not respond to conservative treatment, and at the same time they do not have absolute indications for open surgical intervention. For such cases, PLMD can be effective. However, extensive experience has shown that this method works better in middle-aged patients up to 50 years of age [9]. At the same time, elderly patients are more likely to suffer from DUH. How can we help them? Our experience shows that PLMD can be effective in patients over 50 years of age. However, it is necessary to take into account several conditions.
Material and methods
The work was performed at the Endoscopic Neurosurgery Medical Center in Dnipro, Ukraine, where PLMD has been performed since 1997.
Study participants
The study included 530 patients aged 50 to 72 years, with an average age of 58.6±5.63 years. There were 260 men and 270 women. All patients gave written consent to participate in the research study, as indicated in the outpatient charts. The study was approved by the Ethics and Bioethics Commission of the Dnipro State Medical University of the Ministry of Health of Ukraine
Group characteristics
Out of all 530 patients, 2 groups were formed: group I included patients who underwent PLMD of one or, if necessary, two MHDs, with the presence of protrusions (410), in group II, PLMD was performed on MHD with hernia (120 patients).
Inclusion criteria
The examined group included patients whose age exceeded 50 years, the affected discs retained hydrophilicity and sufficient disc height (not less than 2/3 of the norm), the sagittal size of the herniation did not exceed 6 mm, the absence of ossifying ligamentosis, the absence of degenerative stenosis of the spinal canal, the absence of spondylolisthesis. Protrusions of 3 to 5 mm in size were taken into account
Research design
For the purity of the study, only patients from the last 10 years were selected, in which the Surgilas diode laser (Germany) and the domestic manufacturer – Lika-Surgeon (Cherkasy) was used. The wavelength of the laser was 980 nm. The load on one disk did not exceed 800 J. The duration of one pulse was 1 sec with a load of 15 J. Previously, all patients were examined on magnetic resonance imaging (MRI) machines of various manufacturers, but not lower than the magnetic field strength of 1.5 T. In addition, all patients underwent a computed tomography (CT) scan - a 16-slice tomograph from Toshiba (Japan). The operation was performed under a C-arch fluoroscope from Phillips (Netherlands). Pain was assessed before surgery and within 2 weeks using the VAS scale. The effectiveness of surgery after one month was assessed using the McNab scale.
Statistical analysis
The analysis of the obtained data was carried out using descriptive and analytical biostatistics methods. Quantitative indicators were presented using the arithmetic mean with the standard error (M±m). The magnitude of the treatment effect was calculated using the Cohen (d) method, and its reliability using the student’s t-test for related samples. A p value < 0>
Results and discussion
The neurological condition of the patients was heterogeneous. In patients of group I, the average score of radicular syndromes was 6.4±0.83 according to VAS, and the average score of radicular syndromes was 5.2±0.62 points. Other symptoms occurred in group II: radicular syndrome was 7.24±0.93 points according to VAS, and the average score of radicular syndromes was 4.65±1.43 points. When choosing the tactics of PLD for group II with only symptomatic protrusions, we applied a laser load of about 880 J to the discs from L2 to L5, and about 700 J to the herniated disc L5-S1, taking into account that the volume of this disc is smaller than other discs. In patients of group II with herniated L2-L5 MCD, the laser load was 950 J, and in the case of herniated L5-S1 disc, the laser load was reduced to 750 J.
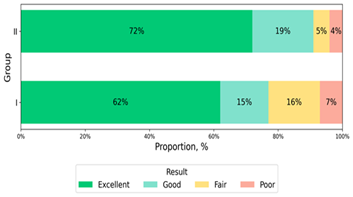
The results of the study (Tabl.No. 1) 1 indicate that in elderly patients of both groups during the first week after PLMD pain increases slightly, which is explained by the aseptic inflammatory reaction of the tissues surrounding the MCD. As for the characteristics of the groups, it can be noted that in group I, patients had symptoms of lumbalgia, while in group II, patients had symptoms of radicular pain. Moreover, the severity of radicular pain was significantly higher than the pain of lumbalgia. By the end of the month, the inflammatory reaction regresses, but the pain still remains at a high level. In group I, radicular pain decreased by only 15%, while in group II, radicular pain decreased by 21%, which is also not very significant. In our opinion, this is due to lower elasticity and lower tendency to repair in elderly patients. According to many scientific studies, in young and middle-aged patients, both radicular pain and lumbalgia significantly decrease a month after PLMD. That is, an elderly patient should be prepared in advance for the fact that after PLMD, the pain syndrome will remain for one month.But this cannot be a contraindication for performing PLMD in elderly patients. Because after 3 months, the condition of such patients has significantly improved, as evidenced by the results of our examination with assessment on the McNab scale. At the same time, it can be noted that in patients of group II, who had hernias, the treatment results were slightly better than in patients of group I (Figure 1).
Table 1: Results of PLM in different groups by pain intensity according to VAS scale
| Pain type | Group | Number of patients | Pain intensity according to VAS | Cohen's d* | ||
| Initial | 1 week later | 1 month later | ||||
| Radicular | І | 410 | 5,2±0,62 | 6,3±0,76 | 4,4±1,43 | -0,04 |
| ІІ | 120 | 7,2±0,93 | 7,8±1,45 | 5,7±0,87 | -0,15 | |
| Lumbalgia | І | 410 | 6,4±0,83 | 7,6±1,24 | 4,2±0,76 | -0,14** |
| ІІ | 120 | 4,65±1,43 | 6,3±0,95 | 3,9±1,24 | -0,05 | |
Notes:* effect size when comparing initial pain intensity with values after 1 month;** significance of treatment effect (p<0>
Figure 1: The condition of patients according to the McNab scale 3 months after PLMD
Thus, despite the fact that the results of PLMD in elderly patients are somewhat worse than in young and middle-aged patients, performing such an operation on them is advisable, given that other treatment methods are ineffective for them. The unsatisfactory results were explained not by technical errors, but by errors in the selection of patients for PLMD.
Conclusions
1. Temporary deterioration of the condition of elderly patients within a month after PLMD is explained by aseptic inflammation of the tissues surrounding the MHD and a decrease in elasticity and a decrease in the tendency to repair in such patients.
2. With the correct selection of elderly patients, PLMD can be quite effective.
Author information
Zorin Mykola, born in 1952. Neurosurgeon, Doctor of Medical Sciences, Professor, Department of Nervous Diseases and Neurosurgery, Dnipro State Medical University. Director of the Medical Center "Endoscopic Neurosurgery"
Discussion
Conflict of Interest
The authors declare no conflict of interest.
Ethical Standards
All procedures performed on patients during the study comply with the ethical standards of the institutional and national ethics committees and the 1964 Declaration of Helsinki
and its later amendments or similar ethical standards.
Informed consent
Informed consent was obtained from each patient.
Funding
The study was not sponsored.
References
- Dobson J. (2019). The marvellous history of medicine. BMJ, 367:l6603.
Publisher | Google Scholor - Tybjerg K. (2022). Scale in the history of medicine. Stud Hist Philos Sci., 91:221-233.
Publisher | Google Scholor - Miziara ID, Miziara CSMG. (2022). Medical errors, medical negligence and defensive medicine: A narrative review. Clinics (Sao Paulo), 77:100053.
Publisher | Google Scholor - Benmoussa N, D'andrea G, Moya-Plana A, Philippe C. Hippocrates (2022). father of mini-invasive nasal surgery. Surg Radiol Anat., 44(10):1375-1378.
Publisher | Google Scholor - REAL ACADEMIA ESPAÑOLA. (2024). Dictionary of the Spanish language, 23rd edition
Publisher | Google Scholor - Keller NC, Schmid S, Hämmerle B (2020). Not every day Caused the Nocturia at dementia Development and Unsteady gait [ On Unusual Reason for Nocturia Combined with Cognitive Decline and Gait Disturbance]. Practice (Bern 1994). 109(15):1201-1204.
Publisher | Google Scholor - Auerbach M, Cole J, Violano P, Roney L, Doherty C, Shepherd M, et al. (2018) International Interprofessional Study of Mental Models and Factors Delaying Neuroimaging of Critically Head-Injured Children Presenting to Emergency Departments. Pediatr Emerg Care, 34(11):797-801.
Publisher | Google Scholor - Shahrizaila N, Lehmann HC, Kuwabara S. (2021). Guillain-Barré syndrome. Lancet, 397(10280):1214-1228
Publisher | Google Scholor - Lurie JM, Png CYM, Subramaniam S, Chen S, Chapman E, et al. (2019). Virchow's triad in silent deep vein thrombosis. J Vasc Surg Venous Lymphat Disord., 7(5):640-645.
Publisher | Google Scholor - Belser-Ehrlich J, Adrian Lafo J, Mangal P, Bradley M, Wicklund M, et al. (2020) Neurocognitive profile of a man with Dandy-Walker malformation: Evidence of subtle cerebellar cognitive affective syndrome. Clin Neuropsychol., 34(3):591-610.
Publisher | Google Scholor - Tan SY, Chong CF, Chong VH. (2020). Charcot's triad. QJM, 113(6):436
Publisher | Google Scholor - Chen JY, Guo ZQ, Wang J, Liu D, Tian E, et al., (2023). Vestibular migraine or Meniere's disease: a diagnostic dilemma. J Neurol., 270(4):1955-1968.
Publisher | Google Scholor - Marrodan M, Fiol MP, Correale J. Susac syndrome. (2022). challenges in the diagnosis and treatment. Brain, 145(3):858-871.
Publisher | Google Scholor - Bongomin F, Khan SA, Oravec T. (2020). A Complete Triad: Horner's Syndrome in Tuberculous Meningitis. Am J Med Sci., 360(2):204-205.
Publisher | Google Scholor - Béreau M, Castrioto A, Lhommée E, Maillet A, Gérazime A, et al., (2022). Fatigue in de novo Parkinson's Disease: Expanding the Neuropsychiatric Triad? J Parkinsons Dis., 12(4):1329-1337.
Publisher | Google Scholor - Pavone P, Polizzi A, Marino SD, Corsello G, Falsaperla R, et al. (2020). West syndrome: a comprehensive review. Neurol Sci., 41(12):3547–3562.
Publisher | Google Scholor - Forst DA, Jones PS. (2023). Skull Base Tumors. Continuum (Minneap Minn)., 29(6):1752–1778.
Publisher | Google Scholor - Zanoletti E, Mazzoni A, Martini A, Abbritti RV, Albertini R, et al. (2019). Surgery of the lateral skull base: a 50-year endeavor. Acta Otorhinolaryngol Ital., 39(SUPPL. 1) :S 1-S146.
Publisher | Google Scholor - Vargas Gálvez CR, López Arbolay O, Ortiz Machín MM. (2024). Minimally invasive approach for Skull -based meningiomas. Neurosurgery (Astur: Engl Ed)., 35(3):127–135.
Publisher | Google Scholor - Vargas Gálvez CR, López Arbolay O, Ortiz Machín MM. (2024). Cranial base reconstruction in patients with olfactory groove meningioma using endoscopic endonasal approaches. Rev Cuban Med Milit, 53(2).
Publisher | Google Scholor - López- Arbolay O, Ortiz-Machín M, Coronado-Rosales A, Menéndez-Palacios M, Solernou -Ferrer A. (2021). Meningiomas of the sellar tubercle. Considerations of the endoscopic endonasal approach. Annals of the Cuban Academy of Sciences, 11(2).
Publisher | Google Scholor - Tritos NA, Miller KK. (2023). Diagnosis and Management of Pituitary Adenomas: A Review . JAMA, 329(16):1386-1398.
Publisher | Google Scholor - Ortiz-Machín M, López- Arbolay O, Goyenechea-Gutiérrez F, Sánchez- Gendriz I. (2022). Extended endoscopic endonasal approach to craniopharyngiomas: the rule of 3 in surgical dissection. Annals of the Cuban Academy of Sciences, 12(3).
Publisher | Google Scholor - Gheorghiu ML, Gheorghisan-Galateanu AA. (2019). CLIVUS CHORDOMA. Acta Endocrinol (Buchar).,15(3):406.
Publisher | Google Scholor - Magill ST, McGahan BG, Carrau RL, Prevedello DM. (2022). Endoscopic endonasal transclival petroclival meningioma resection. Neurosurg Focus Video.,6(2):V 2.
Publisher | Google Scholor - Gezgin I, Yucetas C, Dogan A. (2023). Meningiomas of the Cerebellopontine Angle: Tips and Pearls for Safe Surgical Resection. Turk Neurosurg.,33(3):458-464.
Publisher | Google Scholor - Wang C, Zou Y, Zeng Q, Hong H, Zheng C. (2019). Isolated Rosai-Dorfman disease with craniocervical junction involvement in the foramen magnum: A case report. Medicine (Baltimore)., 98(40): e17433.
Publisher | Google Scholor