Research Article
Point-of-Care Ultrasound Practice: A Perception and Knowledge Assessment Among Pediatrics and Child Health Residents at Two Teaching Hospitals in Addis Ababa, Ethiopia
1Emergency and Critical Care PGY-III Chief Resident at the Department of Emergency and Critical Care, Addis Ababa University, Ethiopia.
2Emergency and Critical Care Consultant at the Department of Emergency and Critical Care, Addis Ababa University, Ethiopia.
3Pediatrics PGY-3 Chief Resident at the Department of Pediatrics and Child Health, Addis Ababa University, Ethiopia.
*Corresponding Author: Robel Sintayehu, Emergency and Critical Care PGY-III Chief Resident at the Department of Emergency and Critical Care, Addis Ababa University, Ethiopia.
Citation: Sintayehu R., Worku T, Feleke Y., Moges M. (2025). Point-of-Care Ultrasound Practice: A Perception and Knowledge Assessment Among Pediatrics and Child Health Residents at Two Teaching Hospitals in Addis Ababa, Ethiopia, Journal of BioMed Research and Reports, BioRes Scientia Publishers. 8(1):1-9. DOI: 10.59657/2837-4681.brs.25.172
Copyright: © 2025 Robel Sintayehu, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: May 06, 2025 | Accepted: May 20, 2025 | Published: May 28, 2025
Abstract
Background: Point-of-care ultrasound is an evolving field in medical education and emergency practice. Numerous pieces of evidence support the use of point-of-care ultrasound in children to improve outcomes. Pediatrics as a specialty has been relatively late to adopt point-of-care ultrasound with a significant gap in specific recommendations and implementation. Assessing pediatrics residents’ perception and knowledge is one of the crucial factors for the successful integration of point-of-care ultrasound into pediatric emergency and critical care practice.
The objective of the study is to describe pediatric residents’ perception towards pediatric point-of-care ultrasound practice and identify factors associated with the knowledge of point of-care ultrasound.
Method: A cross-sectional study assessed the perception and knowledge of 97 pediatric residents from year 1 to year 3 in two tertiary hospitals in Addis Ababa. An online questionnaire was used to collect data on demographics, perception, and knowledge towards point-of-care ultrasound. The data was entered and analyzed using SPSS version 26 software using analytic and descriptive parameters. Binary and multivariable logistic regression analyses were done to identify factors associated with point of care ultrasound knowledge.
Result: Majority (70.1%) of residents have a good understanding of the potential use of point-of-care ultrasound for pediatrics. A majority (67%) of residents rated good perception on point-of-care ultrasound as a valuable tool for improving diagnostic accuracy. On the importance of integrating point-of-care ultrasound training into pediatric residency programs, 70.1% of residents have a good perception. The most significant perceived barrier to point-of-care ultrasound practice is a lack of training (72.2%). Residents with any form of point-of-care ultrasound training were significantly more likely to score above the median knowledge assessment (AOR=58.46; 95% CI: 5.835-585.858; P-value=0.01). Residents who reported using point-of-care ultrasound once a month or once a week were significantly more likely to have a good knowledge of point-of-care ultrasound compared to those who never or rarely used it (AOR= 9.000; 95% CI: 2.307-35.118; P-value=0.020) and (AOR=7.661; 95% CI: 1.375-42.695; P-value=0.039), respectively.
Conclusion and recommendation: Our findings aligned with the broader trend of pediatric residents advocating for the integration of point-of-care ultrasound into pediatric curricula. This integration is likely to increase acceptance among pediatric residents. Our results highlight the importance of prior training and regular use of point-of-care ultrasound in enhancing the knowledge of pediatric residents. We recommend that further studies be conducted to assess the impact of educational interventions on the pre- and post-knowledge of pediatric residents towards point-of-care ultrasound. Another area of interest for future research would be the factors hindering the integration of point-of-care ultrasound into pediatric curricula.
Keywords: point of care ultrasound; pediatrics and child health; residents; addis ababa
Introduction
In pediatric practice, point of care ultrasound allows for rapid, convenient serial reassessments aimed at improving diagnosis. The last two decades have witnessed substantial progress in the development and application of pediatric POCUS. Nevertheless, the advancement has been met with some degree of contention [1]. The first widespread implementation of Pediatric POCUS into practice was urged in 2014 [2]. Following this initiation, a pediatric institutional POCUS training program was conducted in 2015 [3]. In the same year the American Academy of Pediatrics recommended the integration of POCUS training into pediatric emergency fellowships and for physicians [4]. While guidelines for adult patients were published by the Society of Critical Care Medicine in 2015, the European Society for Pediatric and Neonatal Intensive Care has since published comprehensive, evidence-based guidelines [5]. Subsequently, advancements have been made in POCUS training and clinical implementation within both pediatric critical care and emergency medicine settings [6]. A curriculum standard and core POCUS content for PEM fellowships were defined by the Pediatric Emergency Medicine POCUS Network in 2019 [7].
Statement of the problem
Significant uncertainties persist regarding competency standards and training requirements, with variable implementation and adoption. The 2019 national survey found that no pediatric residency programs had a mandatory POCUS curriculum, and less than fifteen percent offered it as an elective [8]. Compared to ten years ago, there has been a notable rise in PEM fellowship training programs, with seventy-seven percent reporting its inclusion in a 2020 survey of program directors [4]. The trend of implementation in more than a hundred surveyed academic pediatric critical care units was found to be low and varied, largely attributed to deficiencies in user training, competence, and confidence [9]. Point of care ultrasound program development emphasizes five key elements: training, credentialing, image storage, documentation, and quality assurance [6]. A significant gap of robust evidence has prevented the establishment of recognized standards for these key components. One survey highlighted a critical deficit of qualified instructors as educators [7]. The rise of Pediatric POCUS has left many questions unanswered, including those related to competency and training.
Significance of the study
In Ethiopia there is no single study which shows the extent of Pediatric POCUS practice and most of the data are inconclusive. Assessing pediatrics residents’ perception and knowledge is one of the crucial factors for the successful integration of point-of-care ultrasound in pediatric emergency and critical care practice. This also aims to serve as an input for stake holder for future implementation and curriculum development. This study assessed pediatric residents’ perception towards pediatric point of care ultrasound practice and identify factors associated with the knowledge of point of care ultrasound.
Literature Review
Point-of-care Ultrasonography is the use of ultrasound imaging by a clinician at the patient's bedside or point of care for immediate diagnostic and therapeutic purposes [2]. This technique will enable the physician to correlate real-time images with the patient’s presenting signs and symptoms [10]. Point-of-care ultrasound can be easily repeated and used for a variety of purposes, including diagnosis and guiding medical procedures [5]. Pediatric emergency and ICU patients often present with ultrasound-detectable abnormalities. It is also an ideal imaging modality for children due to its lack of exposure to radiation and its ability to be performed without sedation [11] A wide range of medical specialties, such as anesthesia, neonatology, internal medicine, family medicine, critical care medicine, and emergency medicine, employ ultrasound [12]. But important to consider, according to the American Academy of Pediatrics policy statement is that “clinicians should be aware that point of care ultrasonography is better used as a rule in and not a rule out diagnostic modality” [13]. In light of the current status, more than seventy percent of fellowship programs in the United States provide formal ultrasound training and less than fifteen percent of residency program offered it as an elective [1] [8]. While various training programs exist, they lack standardized quality assurance and credentialing processes. Additionally, image storage and documentation practices are often inconsistent. While national, regional, and institutional courses are available, they can be costly and limited in accessibility.
The body of literature pertaining to point-of-care ultrasound in the pediatric setting is limited and it is still not well codified. Nevertheless, there aren't many studies that look at how pediatric residents use point-of-care ultrasound. One study conducted with the objective to implement a multi-staged POCUS curriculum and retrospectively assess resident skill and comfort improvement. The curriculum introduced POCUS topics such as basic and advanced cardiac, lung, skin/soft tissues and procedural based ultrasound to all pediatric residents. Study participants demonstrated a thirty percent improvement in POCUS comfort level following the training. It also demonstrated improvement to recognize and interpret POCUS images. Furthermore, all the study participants reported improvement in their practice. This study also highlighted the feasibility of integrating POCUS into pediatric residency training program [12]. In a meta-analysis conducted suggests Pediatric emergency physicians should embrace POCUS as a safe and effective tool for diagnosis, critical care management, and procedural guidance, ultimately enhancing overall patient care [14]. There are several studies which shows about the attitude, level of confidence and comfort of performing Pocus among pediatric residents. According to the studies pediatric residents have little POCUS training and perform poorly on POCUS knowledge testing. While most residents in one study reported a high likelihood of using POCUS in their clinical practice, their confidence levels remained relatively low, particularly in specific scan areas. Nevertheless, all residents agreed that the value of POCUS justified the time investment [15]. A basic POCUS curriculum can be instituted during the PICU and emergency rotation to improve resident knowledge and comfort [16]. Consequently, pediatric emergency and critical care medicine providers will embrace this technology in everyday practice. So far there is no single study or literature found on the trend of POCUS practice in Ethiopia. This gap could be a potential area of study for future in the country. However, one study conducted in Addis Ababa demonstrated that POCUS is the most commonly performed procedure in adult emergency departments [21].
Objective
General Objective: To describe pediatric and child health residents’ perception and knowledge towards point of care ultrasound practice in two teaching hospital in Addis Ababa.
Specific Objectives: To identify factors associated with the knowledge of Pediatric residents towards point of care ultrasound practice. To describe comfort and confidence level of pediatric residents towards point of care ultrasound practice.
Eligibility Criteria
Inclusion criteria: Pediatric Residents should have at least six months of experience in pediatrics department. Pediatric residents should have rotated in ICU or PEM setting.
Exclusion criteria: No POCUS exposure at All. Unable to participate in the study due to serious illness.
Materials and Method
Study Area and Study Period
The study took place in two tertiary hospitals in Tikur Anbessa and St. Paul’s Hospital Millennium Medical specialized hospital located in Addis Ababa, the capital city of Ethiopia. Tikur Anbessa Specialized Hospital is found in the capital city of Addis Ababa and is the largest referral hospital in the country, and serves approximately 370,000- 400,000 patients a year but the exact number is not known. There are 98 residents attending the postgraduate program in the Department of Pediatrics and Child Health at TASH. St. Paul’s Hospital Millennium Medical College, there are 72 residents enrolled in the postgraduate program of pediatrics and child health. It is also located in the capital city of Addis Ababa. The college-initiated Ethiopia’s first integrated modular and problem–based curriculum for its undergraduate medical education and is currently expanding to postgraduate programs including pediatric residency. The study was conducted from May to November/2024 G.C
Study design and Population
A cross-sectional study on pediatric residents’ perception and knowledge towards point of care ultrasound was conducted in two Tertiary hospitals in Pediatrics department. The study was conducted from May to November 2024 G.C. Pediatric Residents from Year 1 to Year 3 at TASH and SPHMMC were included in the study after informed consent was guaranteed.
Source population were all pediatric residents working in Addis Ababa city.
Study population included pediatric residents in two teaching hospitals of Addis Ababa city.
Sampling frame were pediatric residents in two teaching hospitals and participated in the study.
Sample size determination and Sampling Procedure
The required sample size for achieving a 95% confidence interval with a 5% margin of error and proportion of participants with good perception is taken as 50% as there is no similar study done.
The formula for calculating the sample size nn for estimating a single proportion is:
n=Z2⋅p(1−p) d2n=d2Z2⋅p(1−p)
Where:
n = required sample size; Z = Z-value (the number of standard deviations from the mean corresponding to the desired confidence level; for 95% confidence, Z≈1.96Z≈1.96); p = estimated proportion of the population =0.5; d = margin of error = 0.05
n=1.962*0.50(1-0.50)/0.052 = 377
Since the sampling frame is less than 10000, i.e., we use the adjustment formula
nadj.= n/((1+(n/N))
where nadj.= Adjusted sample size; n= calculated sample size; N= Study population
Assuming target population of pediatric residents is approximately 170
nadj.= 384/(1+(384/170))=117
Adjust for Non-response rate is taken as 5%
117*(1/1-NR)= 123
Sampling Procedure – used non-probability sampling (a combination of convenience and quota sampling). The selection of the sample was based on ease of access and convenience. However, to avoid bias and ensure an even distribution of residents from years 1 to 3, a fixed, equal quota was used for each year
Data quality control
The primary investigator, in collaboration with pediatric chief residents, undertook the responsibility of data collection. Before entering the information into the SPSS program, the responses were reviewed daily for completeness of the data.
Methods of data collection and analysis
The data was collected on online questionnaires using a google data collections format from pediatric residents. Assessment questionnaires was provided to assess the perception and knowledge of pediatric residents towards POCUS.All the collected data was organized and analysed by the principal investigator. Study participants' identification was not disclosed to the third party and remained confidential. The questionnaire is prepared in English. Informed consent, in written form, was obtained before physician data collection. Each participant was accessed through their respective hospital. Data was not collected from those physicians who was not cooperative to give consent. The questionnaire included demographics, evaluation of comfort, confidence, perception and knowledge assement. At the end of the questionnaire, a graded knowledge test was provided to the participants. The data was entered and analyzed using SPSS version 26 software using analytic and descriptive parameters. Missing data was treated as missing during analysis. The descriptive data was described using mean with standard deviation, median with interquartile range and mode. Perception and knowledge was assessed using ten questions and twenty questions respectively which was adopted from a previous similar study [17]. The computed median value was used to categorize good and poor perception and knowledge towards POCUS. Since the perception variables were categorical and measured on a Likert scale, they were dichotomized into two groups: above and below the median score. p-value of less than 0.2 in bi-variable analysis were included in multivariable analysis which was conducted to identify factors associated with the level of knowledge towards POCUS. A P-value less than 0.05 was considered statistically significant.
Operational Definitions
Perception: "The belief or opinion that people have as a result of realizing or noticing something"[18].
Good perception towards POCUS: Those who score above the median from perception questions.
Poor perception towards POCUS: Those who score below the median from perception questions.
Good comfort and confidence in POCUS Practice: Those who score above the median from comfort questions.
Bad comfort and confidence in POCUS Practice: Those who score below the median from comfort questions.
Good knowledge of POCUS: Those who score above the median from knowledge questions.
Poor knowledge of POCUS: Those who score below the median from knowledge questions.
Results
The response rate is 78.86% from the calculated sample size. The possible reason for this response rate could be that the study was conducted in the pediatric department and residents were not able to complete the form due to scheduling conflicts and limited availability. However, even with this challenge, the response rate is still quite high.
Sociodemographic
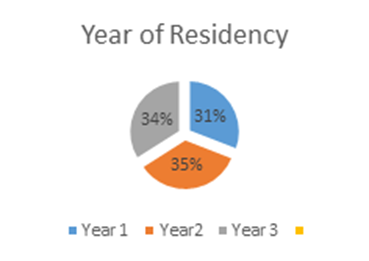
In the study, there were a total of 97 residents, Participants were from Tikur Anbessa Specialized Hospital 54.6%(n=55) and St. Paulo’s Hospital accounted for 45.4% (n=42). The mean age of the study residents is 30.34 years; 95% CI (29.84 to 30.85) with SD of 2.368. The majority of the residents are male (60. 2%). The overall distribution of residents across the three years is relatively even, with a slight predominance of Year 3 residents.
Figure 1
Pediatric Residents' Comfort and Confidence with Pediatric POCUS
The majority of residents (79.4%) reported poor comfort with POCUS practice. A similar trend is observed in self-reported confidence levels, with 78.4% of residents reporting poor confidence to interpret POCUS images. From area of comfort to perform pediatric POCUS, a significant proportion (36.1%) felt uncomfortable with all areas of pediatric POCUS and 35.1 percentage) felt comfortable with IVC POCUS.44.3 percentage of residents never use POCUS in their practice. A significant majority (68%) of residents have not received any formal or informal training in POCUS during their residency program.
Table 1: Comfort and confidence towards pediatric POCUS practice.
| Frequency (%) | 95% CI | |
| Any formal/informal training on POCUS | ||
| Yes | 31(32.0%) | 22.7-41.2 |
| No | 66(68.0%) | 58.8-77.3 |
| Self-reported level of comfort to practice | ||
| Poor | 77(79.4%) | 71.1-87.6 |
| Good | 20(20.6%) | 12.4-28.9 |
| Self-reported level of confidence to interpret POCUS images | ||
| Poor | 76(78.4%) | 69.1-86.6 |
| Good | 21(21.6%) | 13.4-30.9 |
| Area of comfort to perform pediatric POCUS | ||
| FAST Exam | 11(11.3%) | 5.2-17.5 |
| Lung Scan | 14(14.4%) | 7.2-20.6 |
| IVC | 34(35.1%) | 25.8-44.3 |
| Cardiac | 3(3.1%) | 0-7.2 |
| None of it | 35(36.1%) | 26.8-46.4 |
| Self-reported frequency of POCUS practice | ||
| Never | 43(44.3%) | 34.0-54.6 |
| Once a year | 12(12.4%) | 6.2-19.6 |
| Once a month | 14(14.4%) | 7.2-22.7 |
| Once a week | 28(28.9%) | 20.6-37.1 |
Pediatric Residents' Perceptions Towards POCUS Practice
A significant majority (70.1%) of residents have a good understanding on the potential use of POCUS for pediatric patients while 29.9% rated poor. A majority (67%) of residents rated good perception on POCUS as a valuable tool for improving diagnostic accuracy. On the Perception of the importance of Integrating POCUS training to pediatric residency program ,70.1% of residents have good perception. The most significant perceived barrier to POCUS practice is a lack of training (72.2%). The most preferred intervention to improve POCUS proficiency is dedicated practice with an ultrasound machine (40.2%).
Table 2: Perceptions of pediatric residents towards POCUS practice.
| Characteristics | Frequency (Percent) | 95%CI |
| Understanding of the potential use of pediatric pocus for pediatric patients | ||
| Poor | 29(29.9%) | 21.6-39.2 |
| Good | 68(70.1 %) | 60.8-78.4 |
| Perception on use of POCUS for diagnostic accuracy | ||
| Poor | 32(33%) | 23.7-42.3 |
| Good | 65(67%) | 57.7-76.3 |
| Perceived barriers to POCUS practice | ||
| Lack of training | 70(72.2%) | 62.9-81.4 |
| Lack of Equipment | 14(14.4%) | 8.2-21.6 |
| Qualified faculty as educators | 12(12.4%) | 6.2-19.6 |
| Not useful for my patient | 1(1%) | 0-3.1 |
| Perception on the importance of integrating POCUS training to paediatric residency program | ||
| Poor | 29(29.9%) | 20.6-39.2 |
| Good | 68(70.1%) | 60.8-79.4 |
| Perceived intervention to become more proficient on POCUS practice | ||
| Dedicated practice with Ultrasound machine | 39(40.2 %) | 30.9-50.5 |
| Hands on Workshops with simulated scenario | 28(28.8%) | 19.6-40.2 |
| Faculty mentorship for image acquisition and interpretation | 16(16.5%) | 9.3-23.7 |
| Didactic lectures on POCUS applications | 11(11.3%) | 5.2-17.5 |
| Access to online learning modules | 3(3.1%) | 0-7.2 |
Factors Contributing to Pediatric Residents' Knowledge of POCUS
A total of 49(51%) of residents below the median on the POCUS exam, while 47(49%) residents scored above the median. This suggests that the majority of residents achieved a score below the lower threshold. Year 1 residents had the highest proportion (77%) scoring below the threshold. Year 3 residents had the highest proportion (73%) scoring above the threshold. 17 residents (52%) from year 2 Scored above the median. Residents with previous POCUS training were significantly more likely to score above the median POCUS score with the AOR 58.46 (95% CI: 5.835-585.858), indicating a strong positive association between training and POCUS knowledge. Residents in Year 2 and Year 3 were found to have a higher likelihood of having a good knowledge of POCUS compared to Year 1 residents. Residents who reported using POCUS once a month or once a week were significantly more likely to have a good knowledge of POCUS compared to those who never or rarely used it.
Table 3: Factors Contributing to the Knowledge of Pediatric residents toward Pediatric POCUS application.
| Score of POCUS Questions | ||||||
| Characteristics | Good | Poor | COR95%CI | AOR 95%CI | P-Value | |
| Sex | Female | 20(20.83%) | 18(18.75%) | Reference | Reference | |
| Male | 27(28.13%) | 31(32.3%) | 0.784(0.345-1.770) | 0.447(0.112-1.783) | 0.254 | |
| Age | 26-29 | 16(18.18%) | 21(23.86%) | Reference | Reference | |
| 30-33 | 21(23.86%) | 15(17.04%) | 1.837(0.726-4.650) | 1.173(0.283-4.857) | 0.826 | |
| 34-37 | 5(5.68%) | 10(11.36%) | 0.656(0.187-2.302 | 0.512(0.069-3.826) | 0.514 | |
| Institution | St. Paulo’s | 20(23.95%) | 22(19.79%) | Reference | Reference | 0.153 |
| TASH | 27(25%) | 26(31.25%) | 1.648(0.732-3.708) | 3.305(0.642-17.023) | ||
| Previous POCUS training | No | 18(18.75%) | 47(48.95%) | Reference | Reference | 0.01 |
| Yes | 29(30.20%) | 2(2.08%) | 58.46(5.835-585.858) | 37.861(8.178-175.275) | ||
| Year of Residency | Year 1 | 7(7.29%) | 23(23.95%) | Reference | Reference | |
| Year 2 | 17(17.7%) | 16(16.66% | 3.092(1.043-9.171) | 7.061(0.804-62.04) | 0.078 | |
| Year 3 | 24(25%) | 9 (9.37%) | 8.762(2.798-27.434) | 8.254(0.968-70.373) | 0.054 | |
| Self-reported frequency of POCUS practice | Never | 7(7.29%) | 35(36.45%) | Reference | Reference | |
| Once a year | 6(6.25%) | 6(6.625% | 5.000(1.24-20.124) | 3.634(0.671-19.785) | 0.134 | |
| Once a month | 9 (9.37) | 5(5.2%) | 9.000(2.307-35.118) | 7.661(1.375-42.695) | 0.02 | |
| Once a week | 25(26.04%) | 3((3.12%) | 57.5(10.964-301.562) | 14.386(1.138-181.927) | 0.039 | |
Discussion
The objective of this study is to describe pediatric residents’ perception towards pediatric point of care in government teaching hospitals in Addis Ababa, Ethiopia; to identify factors associated with the knowledge of point of care ultrasound in two teaching government hospitals in Addis Ababa. In this study findings, the majority of residents have a good understanding of the potential use of POCUS for pediatric patients. As well, they rated well on perception of POCUS as a valuable tool for improving diagnostic accuracy, on the potential use of POCUS for pediatric patients, and on the importance of integrating POCUS training into the pediatric residency program. A significant majority of residents (79.4%) reported poor comfort and confidence with POCUS practice and interpretation of POCUS images. Residents with any form of POCUS training were more likely to score above the median POCUS knowledge assessment with a statistical significance. But a significant majority (68%) of residents have not received any formal or informal training in POCUS during their residency program. Another statistically significant finding of the study was residents who reported using POCUS once a month or once a week were more likely to have a good knowledge of POCUS compared to those who never or rarely used it. Residents in Year 2 and Year 3 were also found to be marginally significant likelihood of having a good knowledge of POCUS compared to Year 1 residents.
Our study suggests that pediatric residents not only understand potential use of POCUS but also regard it as crucial for enhancing diagnostic accuracy .As well, They rated well on the importance of integrating POCUS training into the pediatric residency program This is supported by a national survey indicating that 96% of pediatric trainees believe POCUS is an important skill in pediatrics, with 92 percentage advocating for its inclusion in residency training programs [19] .Similar study found that 56% of pediatric residency program directors felt that all residents should be trained in POCUS, reflecting a widespread acknowledgment of its value in clinical practice. While our findings emphasize a positive perception of POCUS, they also underscore the need for structured training programs. In line with this, a study conducted at the University of Catania reported that 100% of participants expressed the necessity for formal POCUS training within their residency curriculum [20]. These parallels our results showing that residents rated the integration of POCUS training as important for their education. Despite the favorable attitudes towards POCUS, barriers to effective training persist. Our study reflected that the most perceived barrier by pediatric residents to POCUS practice is a lack of training (72.2%), similar challenges was noted in other research, where 94% of pediatric residency program directors cited a lack of qualified instructors as a significant obstacle to implementing POCUS training[1] [19, 20].
The finding from our study showed only thirty-two percent of pediatric residents had received previous training in POCUS, whether informal, such as bedside training, or formal. On a national need assessment survey reveal variability in how this training is implemented across different residency programs. For instance, some programs offer informal bedside education, only 37% provide any formal POCUS training [9]. Pediatric residents with any form of POCUS training were more likely to score above the median POCUS knowledge assessment which is statistically significant as reflected in our study. For instance, a study conducted at a large children's hospital found that after a two-week POCUS course, residents demonstrated significant improvements in self-reported confidence and knowledge across various POCUS competencies, including image acquisition and interpretation (P less than 0.01) [17]. In addition, the majority of our participants reported poor comfort with point-of-care ultrasound (POCUS) practice and rated poor confidence in interpreting POCUS images, Thus, prior exposure to POCUS training can enhance both comfort and knowledge levels among pediatric residents. Another statistically significant finding associated with POCUS knowledge is self-reported frequency of practice and using point-of-care ultrasound (POCUS) once a month or once a week were significantly more likely to have good knowledge of POCUS compared to those who never or rarely used it. The relationship between the frequency of POCUS use and self-reported confidence is well-documented in another research. A study conducted on pediatric residents showed that those who regularly utilized POCUS in clinical settings felt significantly more confident in their skills compared to those with limited exposure. This aligns with our findings, as residents using POCUS weekly or monthly had markedly better knowledge scores than those who rarely or never used it [12, 20].
Conclusion and recommendation
Our results highlight the importance of prior training and regular use of point of care ultrasound in enhancing the knowledge of pediatric residents. These factors are crucial for the successful implementation of point of care ultrasound in pediatric training programs. While there is a clear recognition of the value of POCUS training, addressing barriers to effective implementation will be essential for maximizing its benefits in pediatric education. Developing comprehensive curricula that emphasize hands-on experience could significantly improve both resident competence and patient care outcomes in pediatric settings. We recommend that further studies be conducted to assess the impact of educational interventions on the pre- and post-knowledge of pediatric residents towards point of care ultrasound. Another area of interest for future research would be the factors hindering the integration of point-of-care ultrasound into pediatric curricula.
Limitation and strength of the study
The strength of this study is that it is the first of its kind in Ethiopia to explore this specific aspect. Although selection bias could not be avoided as the method used is convenience sampling method, the study's objective was to get a better understanding through exploration of the barriers to POCUS practice in pediatric and child health department in the selected teaching hospitals. The other limitations of our study are the discrepancy between the actual sample size of the participants and the calculated sample size, which was due to a high rate of non-response, and the fact that the study was conducted in only two teaching hospitals. This may limit the generalizability of our findings to the broader population.
Acronyms and Abbreviation
ACEP--American College of Emergency Physician; AAP--American Academy of Pediatrics; AAU –Addis Ababa University; AOR--Adjusted Odds ratio; COR--Crudes Odds ratio; CI--Confidence interval; ED--Emergency Department; EFAST--Extended Focused Assessment with Sonography for Trauma; ESPNIC-- European Society of Pediatric and Neonatal Intensive Cares; FAST-- Focused Assessment with Sonography for Trauma; PEM--Pediatric Emergency Medicine; PICU--Pediatric Intensive Care Unit; POCUS--Point-of-care ultrasonography; SD--Standard deviation; SPHMMC--St.Paulos Hospital Millennium Medical College; TASH--Tikur Anbessa Specialized Hospital
Declarations
Ethical clearance and participant consent
This study was conducted in accordance with the Declaration of Helsinki. Permission to conduct the study was granted by institutional ethical committees from the Addis Ababa University emergency department. under College of Health Sciences Institutional Review Board (Ref. No. 559/2015).
Consent for publication
Not applicable
Availability of data and materials
The data sets used and analyzed in this study are available from the corresponding author on reasonable request.
Conflict of interest
None of the authors has any competing interest to disclose. We confirm that we have read the Journal’s position on issues involved in ethical publication.
Funding
There was no source of funding in any form or organization.
Author Contributions
Statement: R.S.- served as the principal investigator of this study and was responsible for developing the proposal, conceptual framework, and data collection tools before the study commenced. During the study, he conducted data collection, performed data analysis, and wrote the majority of the manuscript. He also prepared the tables for the publication. T.W.'s and Y.F. 's primary role throughout the study was to provide advice and guidance from its inception. They offered technical support, assisted with data analysis, and supervised the overall study's progress. Revising the manuscript, providing valuable feedback, and giving corrections. M.G. was involved in this study from its inception, contributing to the development of the proposal. He actively participated in data collection and analysis and provided significant assistance with the writing of this manuscript, particularly the results section. All authors reviewed the manuscript.
Acknowledgments
We would like to thank Professor Aklilu for their relentless motivation throughout the research process and A special thanks to Ms. Eden for her significant contributions to the preparation of the tables and figures.
References
- Burton, L., Bhargava, V., & Kong, M. (2022). Point-of-care ultrasound in the pediatric intensive care unit. Frontiers in Pediatrics, 9:830160.
Publisher | Google Scholor - Su, E., Pustavoitau, A., Hirshberg, E. L., Nishisaki, A., Conlon, T., Kantor, D. B., et al. (2014). Establishing intensivist-driven ultrasound at the PICU bedside—It's about time. Pediatric Critical Care Medicine, 15:649–652.
Publisher | Google Scholor - Conlon, T. W., Himebauch, A. S., Fitzgerald, J. C., Chen, A. E., Dean, A. J., Panebianco, N., et al. (2015). Implementation of a pediatric critical care focused bedside ultrasound training program in a large academic PICU. Pediatric Critical Care Medicine, 16:219–226.
Publisher | Google Scholor - Acuña, J., Rubin, M., Hahn, B., et al. (2020). Point-of-care ultrasound in United States pediatric emergency medicine fellowship programs: The current state of practice and training. Pediatric Emergency Care.
Publisher | Google Scholor - Singh, Y., Tissot, C., Fraga, M. V., Yousef, N., Cortes, R. G., et al. (2020). International evidence-based guidelines on point-of-care ultrasound (POCUS) for critically ill neonates and children. Critical Care, 24:65.
Publisher | Google Scholor - Conlon, T. W., Kantor, D. B., Su, E. R., Basu, S., Boyer, D. L., Haileselassie, B., et al. (2018). Diagnostic bedside ultrasound program development in pediatric critical care medicine: Results of a national survey. Pediatric Critical Care Medicine, 19, e561–e568.
Publisher | Google Scholor - Shefrin, A. E., Warkentine, F., Constantine, E., et al. (2019). Consensus core point-of-care ultrasound applications for pediatric emergency medicine training. AEM Education and Training, 3(3):251–258.
Publisher | Google Scholor - Reaume, M., Siuba, M., Wagner, M., Woodwyk, A., & Melgar, T. A. (2019). Prevalence and scope of point-of-care ultrasound education in internal medicine, pediatric, and medicine-pediatric residency programs in the United States. Journal of Ultrasound in Medicine, 38(6):1433–1439.
Publisher | Google Scholor - Lambert, R. L., Boker, J. R., & Maffei, F. A. (2011). National survey of bedside ultrasound use in pediatric critical care. Pediatric Critical Care Medicine, 12:655–659.
Publisher | Google Scholor - De Souza, T. H., Brandao, M. B., Nadal, J. A. H., & Nogueira, R. J. N. (2018). Ultrasound guidance for pediatric central venous catheterization: A meta-analysis. Pediatrics.
Publisher | Google Scholor - Marin, J. R., Abo, A. M., Arroyo, A. C., et al. (2016). Pediatric emergency medicine point-of-care ultrasound: Summary of the evidence. Critical Ultrasound Journal, 8:16.
Publisher | Google Scholor - Brant, J. A., Orsborn, J., Good, R., Greenwald, E., Mickley, M., & Toney, A. G. (n.d.). Evaluating a longitudinal point-of-care-ultrasound (POCUS) curriculum for pediatric residents. PubMed.
Publisher | Google Scholor - Díaz-Gómez, J. L., Mayo, P. H., & Koenig, S. J. (2021). Point-of-care ultrasonography. New England Journal of Medicine, 385(17):1593–1602.
Publisher | Google Scholor - Le Coz, J., Orlandini, S., Titomanlio, L., & Rinaldi, V. E. (2018). Point-of-care ultrasonography in the pediatric emergency department. Italian Journal of Pediatrics, 44(1):87.
Publisher | Google Scholor - Willis, E., Finn, E., Dancel, R., & Park, D. (n.d.). Pediatric point-of-care ultrasound (POCUS) residency curriculum.
Publisher | Google Scholor - Good, R., Orsborn, J., & Stidham, T. (2018). Point-of-care ultrasound education for pediatric residents in the pediatric intensive care unit. MedEdPORTAL, 14:10683.
Publisher | Google Scholor - Arichai, P., Delaney, M., Slamowitz, A., Rosario, R., Gordish-Dressman, H., Basu, S., et al. (2022). Pediatric residency point-of-care ultrasound training needs assessment and educational intervention. Cureus, 14(9):e28696.
Publisher | Google Scholor - Sinclair, J. (Ed.). (1994). Collins COBUILD English language dictionary (7th repr.). Harper Collins.
Publisher | Google Scholor - Good, R. J., O’Hara, K. L., Ziniel, S. I., Orsborn, J., Cheetham, A., & Rosenberg, A. (2021). Point-of-care ultrasound training in pediatric residency: A national needs assessment. Hospital Pediatrics, 11(11):1246–1252.
Publisher | Google Scholor - Lo Bianco, M., Presti, S., Finocchiaro, M. C., Trobia, G. L., Sciacca, T. V., Cucuzza, M. E., et al. (2024). Point-of-care ultrasound (POCUS) pediatric resident training course: A cross-sectional survey. Italian Journal of Pediatrics, 50(1):82.
Publisher | Google Scholor - Zewdie, A., Abicho, T., Alemu, D., & Aspler, A. (2023). Point-of-care ultrasound (POCUS) utilization and barriers by senior emergency medicine and critical care residents at two teaching referral hospitals, Addis Ababa, Ethiopia. Emergency Medicine International, 2023.
Publisher | Google Scholor