Case Report
Isolated Omental Tears as a Rare Source of Massive Hemoperitoneum Following Blunt Abdominal Trauma: A Case Report
- Gurmeet Singh Sarla *
- Narendra Chetri
- Samrat Sunkar
General and Laparoscopic Surgeon, Department of Surgery, Military Hospital Khadki, Pune, Maharashtra, India.
*Corresponding Author: Gurmeet Singh Sarla, General and Laparoscopic Surgeon, Department of Surgery, Military Hospital Khadki, Pune, Maharashtra, India.
Citation: Sarla GS, Chetri N, Sunkar S. (2025). Isolated Omental Tears as a Rare Source of Massive Hemoperitoneum Following Blunt Abdominal Trauma: A Case Report, International Journal of Biomedical and Clinical Research, BioRes Scientia Publishers. 4(5):1-3. DOI: 10.59657/2997-6103.brs.25.095
Copyright: © 2025 Gurmeet Singh Sarla, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: September 17, 2025 | Accepted: October 31, 2025 | Published: November 07, 2025
Abstract
Background: Blunt abdominal trauma typically results in injury to solid organs, most commonly the liver and spleen. Injuries to the omentum are rare but may lead to life-threatening hemoperitoneum, often evading detection during initial operative exploration.
Case Presentation: A 49-year-old man presented in hemorrhagic shock after blunt abdominal trauma. Focused abdominal ultrasonography revealed free intraperitoneal fluid. Emergency laparotomy evacuated approximately 2.5 L of blood and clots. No major solid organ injury was identified; however, systematic exploration revealed large tears in the lesser (8 × 6 cm) and greater (12 × 8 cm) omentum with active bleeding. The defects were repaired using fresh omental patches and ligation of bleeding vessels. The postoperative course was uneventful.
Conclusion: Isolated omental tears, although uncommon, can be a significant source of hemoperitoneum. In the absence of solid organ injury, surgeons should maintain a high index of suspicion and perform careful intra-operative exploration to achieve timely hemostasis.
Keywords: blunt abdominal trauma; omental tear; hemoperitoneum; exploratory laparotomy; omental patch
Introduction
Blunt abdominal trauma continues to be a major contributor to morbidity and mortality globally and remains a frequent indication for emergency laparotomy [1,2]. Most intra-abdominal bleeding arises from solid organ injuries, particularly the liver and spleen [1-3]. By contrast, isolated omental injuries are uncommon, representing only a small proportion of traumatic hemoperitoneum cases [4-6].
The omentum receives its blood supply from the gastroepiploic arteries and their branches, forming a rich vascular network. Disruption of these vessels can lead to rapid and substantial bleeding [2,4]. Because of the omentum’s mobility, injuries may not be immediately evident and can be concealed by clots or adjacent viscera [5,6]. In patients who are hemodynamically unstable, preoperative imaging is often not feasible, making meticulous intra-operative assessment critical.
We report a rare instance of isolated omental tears resulting in massive hemoperitoneum following blunt trauma, emphasizing the importance of systematic exploration and timely surgical management.
Case Presentation
A 49-year-old man presented to the emergency department following blunt abdominal trauma. He was restless and in hemorrhagic shock, with blood pressure 80/50 mmHg, heart rate 130/min, respiratory rate 28/min, and SpO₂ 90% on room air. Laboratory evaluation revealed hemoglobin 7.0 g/dL, platelet count 1.8 × 10⁵/µL, INR 1.3, and creatinine 0.9 mg/dL. Extended focused abdominal sonography demonstrated free intraperitoneal fluid.
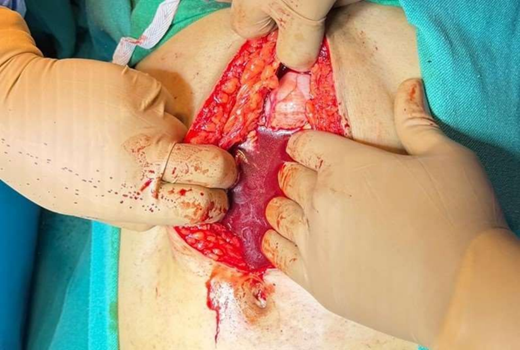
Following rapid fluid resuscitation, the patient underwent emergency midline laparotomy. Approximately 1.5 L of fresh blood and 1.0 L of clots were evacuated. No significant injury to the liver, kidneys, or hollow viscera was observed. Persistent bleeding prompted quadrant-wise inspection, revealing an 8 × 6 cm tear in the lesser omentum and a 12 × 8 cm tear in the greater omentum, both actively bleeding. A minor 0.5 cm splenic capsular tear was noted but not actively bleeding.
Hemostasis was achieved by ligating bleeding omental vessels and repairing the tears with fresh omental patches. The peritoneal cavity was irrigated thoroughly. Drains were placed in Morrison’s pouch, the splenorenal recess, and the pelvis. Intra-operative transfusion included 2 units of packed red blood cells and 4 units of fresh frozen plasma.
Postoperatively, the patient’s hemodynamics stabilized within 24 hours. Drain output decreased progressively from 40 mL on postoperative day (POD) 1 to less than 30 mL by POD 3, and hemoglobin improved to 10 g/dL by POD 3. He was mobilized on POD 1, resumed oral intake on POD 2, and drains were removed sequentially between POD 4 and 7. The patient was discharged in stable condition.
Discussion
Omental hemorrhage is an uncommon etiology of hemoperitoneum, with most cases arising from trauma, vascular anomalies, neoplasms, or coagulopathies [5-8]. Within traumatic causes, isolated omental tears are particularly rare, contributing minimally to overall intra-abdominal bleeding [6,7].
Mechanisms of Injury: Blunt trauma can cause omental tears through several mechanisms. Direct compression against the abdominal wall may rupture the omental vascular arcade. Sudden deceleration can generate shearing forces at the points of vascular attachment, and traction may tear the mobile greater omentum [2,4]. Due to its size and exposure, the greater omentum is more frequently affected, although lesser omental tears, as in this case, can also produce significant hemorrhage due to the caliber of gastroepiploic vessels.
Diagnostic Considerations: In hemodynamically stable patients, CT imaging can detect omental hematomas, active contrast extravasation, or focal masses indicative of bleeding [5,9]. In unstable patients, bedside ultrasound identifies free fluid but cannot reliably determine the bleeding source. This limitation underscores the need for careful intra-operative evaluation. Literature reports frequently cite missed omental injuries at initial inspection, often revealed only after thorough lavage and systematic quadrant-wise exploration [6,7]. Our case mirrored this, with the source identified only after meticulous intra-operative assessment.
Management Strategies: Treatment depends on hemodynamic status. In unstable patients, operative intervention is the standard of care, consistent with ATLS recommendations [10]. Surgical options include ligation of bleeding vessels, partial omentectomy, or repair using fresh omental patches [1-3]. In select stable patients with vascular lesions such as omental artery aneurysms, transcatheter arterial embolization may be considered [9]. Damage-control approaches are warranted in patients with coagulopathy, hypothermia, and acidosis [2,10].
Key Learning Points
- Massive hemoperitoneum in the absence of solid organ injury should prompt consideration of rarer sources, such as the omentum.
- Quadrant-wise exploration and thorough removal of clots are essential to identify active bleeding.
- Omental patch repair with vessel ligation is effective and preserves omental tissue, while segmental omentectomy may be necessary for complex injuries.
- Early recognition and adherence to ATLS protocols improve outcomes in unstable trauma patients.
Conclusion
Although uncommon, isolated omental tears can result in significant hemoperitoneum following blunt abdominal trauma. Surgeons should maintain a high index of suspicion when no solid organ injury is evident. Prompt operative exploration, meticulous quadrant-wise inspection, and timely hemostasis via vessel ligation, patch repair, or omentectomy are critical for successful management.
References
- Townsend, C. M., Beauchamp, R. D., Evers, B. M., Mattox, K. L. (2016). Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. Elsevier Health Sciences.
Publisher | Google Scholor - Bailey, H., Bulstrode, C. J., O'Connell, P. R. (2008). Bailey & Love's Short Practice of Surgery. Crc Press.
Publisher | Google Scholor - Seymour I. Schwartz. Principles of Surgery: Redux and Reconsideration. 11th Edition. McGraw Hill.
Publisher | Google Scholor - Skandalakis, J. E. (2004). Skandalakis' Surgical Anatomy: The Embryologic and Anatomic Basis of Modern Surgery (Vol. 2). PMP.
Publisher | Google Scholor - Zissin R, Hertz M, Gayer G, et al. (2001). Traumatic Injuries of The Omentum: CT Findings. Emerg Radiol. 8(6):295–299.
Publisher | Google Scholor - Kimura, J., Okumura, K., Katagiri, H., Lefor, A. K., Mizokami, K., et al, T. (2016). Idiopathic Omental Hemorrhage: A Case Report and Review of The Literature. International Journal of Surgery Case Reports, 28:214-218.
Publisher | Google Scholor - Lyu, Y. X., Cheng, Y. X., Li, T. (2018). Spontaneous Omental Bleeding: A Case Report and Literature Review. BMC Surgery, 18(1):33.
Publisher | Google Scholor - Rashidi, F., Samimiat, A., Jafarimehrabady, N., Hajebi, R. (2023). Idiopathic Omental Hemorrhage: A Case Report and Review of The Literature. Journal of Medical Case Reports, 17(1):368.
Publisher | Google Scholor - Maghrebi, H., Zaiem, A., Beji, H., Jeribi, B., Hadded, A., et al. (2022). Spontaneous Rupture of a Left Omental Artery Aneurysm Treated by Transcatheter Arterial Embolization: A Case Report. Annals of Medicine and Surgery, 82.
Publisher | Google Scholor - American College of Surgeons. (2018). ATLS: Advanced Trauma Life Support. 10th ed. Chicago: ACS.
Publisher | Google Scholor