Research Article
Clinical Performance of Roughened Single-Piece Zirconia Dental Implants: A Retrospective Case Series
- Dr. Chirag Chamria
- Dr. Jemmie Joy Alexander*, BDS *
Oral & Maxillofacial Surgeon, MDS Royal Dental Clinics, Mumbai, India.
*Corresponding Author: Dr. Chirag Chamria, Oral & Maxillofacial Surgeon, MDS Royal Dental Clinics, Mumbai, India.
Citation: Chamria C., Jemmie J. Alexander. (2026). Clinical Performance of Roughened Single-Piece Zirconia Dental Implants: A Retrospective Case Series, Clinical Case Reports and Studies, BioRes Scientia Publishers. 12(1):1-6. DOI: 10.59657/2837-2565.brs.26.294
Copyright: © 2026 Jemmie Joy Alexander, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: December 02, 2025 | Accepted: December 19, 2025 | Published: January 07, 2026
Abstract
Background: Zirconia dental implants are a metal-free alternative to titanium with potential advantages in aesthetics, soft-tissue biocompatibility, and plaque affinity. Systematic reviews report high long-term survival for one-piece zirconia implants, while two-piece systems show more variable early outcomes [1–3]. However, practice-based longitudinal data with ceramic-specific insertion protocols remain limited.
Objective: To evaluate clinical survival and complication patterns of roughened single-piece zirconia implants placed, including a post-radiotherapy subset.
Materials and Methods: This retrospective case series included 32 implants placed in 12 patients. Clinical success was defined as absence of mobility, persistent pain, chronic infection, or prosthetic failure. A zirconia-specific surgical protocol was used, emphasizing condensation-based osteotomy, low-speed instrumentation, and controlled torque (15 Ncm machine torque → ≥25 Ncm hand torque). A minimum follow-up of 6 months was required for inclusion in the survival analysis.
Results: Of 32 implants, 31 had ≥ 6 months follow-up. Four failures occurred (12.5%), all in the lower right posterior mandible, giving a survival rate of 87.5%. Two failures occurred in a fibula-reconstructed irradiated mandible. The remaining irradiated patient exhibited 5 stable implants. Narrow diameters (2.5 mm) and high-load posterior sites showed the greatest susceptibility to failure. Narrow-diameter implants (2.5–3.0 mm) dominated the cohort, consistent with literature identifying fracture and early failure risks in narrow zirconia implants [1,4].
Conclusion: When placed using zirconia-specific techniques, roughened single-piece zirconia implants demonstrate acceptable survival and favourable soft-tissue behaviour, even in selected irradiated jaws. Host-bone biology—particularly reconstruction and irradiated segments—plays a dominant role in determining survival. The results support routine use of single-piece zirconia implants in aesthetic and standard cases, with cautious application in high-risk posterior mandibular and reconstructed segments.
Keywords: zirconia implants; ceramic implants; one-piece implants; roughened surface; post-radiotherapy jaw; implant survival; case series
Introduction
Zirconia dental implants have gained clinical traction due to increasing demand for metal-free rehabilitation and improved peri-implant soft-tissue esthetics. Contemporary zirconia systems exhibit high flexural strength and fracture toughness, and surface roughening strategies have improved osseointegration predictability.1,5 Systematic reviews and consensus statements show that zirconia implants can achieve survival rates comparable to titanium, particularly for commercially available one-piece designs [1–3,6]. A large 2023 meta-analysis estimated a 10-year cumulative survival of 95% for zirconia implants, with one-piece designs outperforming two-piece systems [1]. The ITI consensus also supports one-piece zirconia implants in appropriate clinical conditions while advising caution with two-piece systems because of inconsistent evidence.6 Modern meta-analyses estimate 95–97% survival at 5–10 years in non-complex cases.
Biologically, zirconia is associated with low plaque affinity and favorable mucosal responses, potentially reducing inflammatory burden [3,7]. In esthetic zones, zirconia’s tooth-colored core avoids gray shine-through in thin biotypes [8]. Zirconia may also be advantageous in complex host conditions, including irradiated jaws, where biocompatibility and reduced corrosion/ion release are desired [9]. Although survival data in irradiated bone are still evolving, implant survival in head-and-neck oncology cohorts depends strongly on radiation dose, vascularity, and reconstruction type [9,10].
In routine practice, ceramic implants require torque-appropriate protocols. Excessively high insertion torque may risk micro-crack propagation or crestal ischemia [4,11]. Seldom cases of implant fracture are also noted. Therefore, clinical case series describing real-world insertion strategies and long-term stability are important to guide safe adoption.
This retrospective case series presents outcomes of roughened single-piece zirconia implants placed, including performance in two anonymous post-radiotherapy patients.
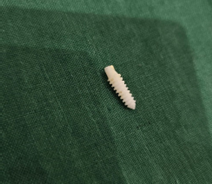
Figure 1: zirconia implant
Materials and Methods
Study design and setting
A retrospective case series was performed at private dental clinic in India, including all consecutive cases rehabilitated with roughened single-piece zirconia implants. The report follows STROBE principles for observational studies.
Inclusion criteria
- Adults ≥18 years.
- Single-piece zirconia implants placed for single-tooth replacement or segmental rehabilitation.
- Minimum clinical follow-up of 6 months for inclusion in survival analysis.
Exclusion criteria
- Patients with uncontrolled systemic disease at time of surgery.
- Active untreated generalized periodontitis.
- Incomplete clinical records preventing outcome determination.
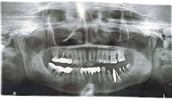
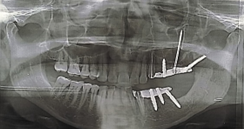
Figure 2: 2 zirconia implants in the 4th quadrant posteriorly.
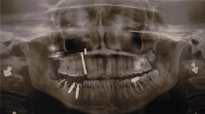
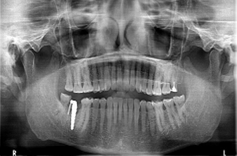
Figure 3: OPG of zirconia implant in one of our patients
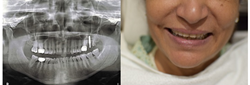
Figure 4: OPG [1 zirconia implant placed in #27] and clinical photograph
Implant system
- Material: Zirconium dioxide ceramics.
- Design: Single-piece.
- Surface: Roughened (macro- and micro-textured) to enhance bone-implant contact [1,5].
- Diameters used in this cohort: 2.5 to 4.0 mm.
- Lengths categories: <15mm>20mm.
Surgical protocol
The osteotomy and insertion technique were adapted for ceramic biomechanics:
- Atraumatic access: crestal mini-flap or flapless approach when anatomy allowed.
- Pilot drilling under copious irrigation to limit thermal insult.
- Sequential drilling with emphasis on bone condensation; final osteotomy maintained 0.5 mm undersized relative to implant diameter.
- A bone-condensation drill was used at low speed and subsequently reversed in a controlled manner to preserve the integrity of the native bone threads.
- Torque limitation strategy:
- Machine-driven seating at 15 Ncm to near-final depth.
- Manual driver finishes to ≥ 25 Ncm for controlled final seating.
- Avoidance of over-torquing given zirconia’s susceptibility to stress concentration and the recognized link between narrow zirconia implants and fracture/early failure [1,4].
- Immediate temporization only when clinical stability was deemed sufficient by tactile and torque criteria.
Clinical rationale
Zirconia implants were inserted at lower torque targets than titanium systems because primary stability is predominantly achieved through a bone-condensation effect rather than high compressive torque. Controlled insertion minimizes ceramic micro-stress and crestal ischemia.4,11
Prosthetic protocol
- Interim prostheses were provided in stable cases.
- Final restorations were delivered in functional occlusion with attention to load distribution; occlusion was checked clinically and with digital occlusal assessment when indicated.
- Cementation was performed with strict excess-cement control to reduce peri-implant inflammation risk [12].
Follow-up and outcome criteria
Patients were recalled at 1 week, 1 month, 3 months, 6 months, 12 months, and annually thereafter. All patients remain under ongoing follow-up.
Because standardized marginal bone loss (MBL) measurements were not captured, outcomes were assessed via clinical success:
- Absence of mobility
- Absence of persistent pain
- Absence of suppuration or recurrent infection
- Functional stability under prosthetic loading
This approach aligns with commonly reported clinical success endpoints when radiographic quantification is unavailable [3].
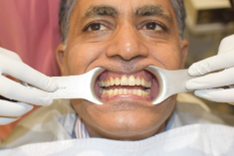
Figure 5: patient clinical picture
Figure 6: OPG of the same patient 1 zirconia implant placed in #47
Statistical analysis
Descriptive statistics were computed for implant distribution, survival, and failure pattern. Survival was calculated as implants retained in function without clinical mobility at ≥ 6 months.
Results
Study population
- Patients: 12
- Implants placed: 32
- Analytic survival cohort (≥6 months): 31
- One implant placed on Nov 2025 had less than 6-month follow-up and was excluded from survival calculations but remains clinically stable to date.
- Failure 4:
- Survival Rate: 87.5%
These patterns reflect frequent use of narrow and long implants, consistent with posterior mandibular rehabilitation and reconstructed segments.
Failure pattern
Four failures were recorded:
- All failures occurred in the lower right posterior region.
- Two failures occurred in a single irradiated fibula-reconstructed mandible (Patient R1) and were annotated as reconstruction-related failures.
- The remaining two failures were posterior mandibular cases without reconstruction annotation.
Discussion
This retrospective series of roughened single-piece zirconia implants demonstrates acceptable real-world survival (87.1%) with up to 5-year follow-up. Published evidence indicates that modern zirconia implants, particularly one-piece designs, can reach 5- to 10-year survival around 95–97% in healthy cohorts.1–3,6 The survival observed here is lower than pooled estimates, likely reflecting case-mix complexity, narrow-diameter usage, and irradiated /reconstructed host bone.
One-piece zirconia designs and survival
Large systematic reviews show that one-piece zirconia implants outperform two-piece systems, with two-piece designs reporting higher early losses and prosthetic biomechanical challenges [1,2,6]. Recent prospective data on certain two-piece zirconia systems demonstrate low 12-month survival, underscoring the importance of implant selection and design-specific evidence [2,13]. Our cohort exclusively used single-piece implants, aligning with current consensus for predictable ceramic implantology [6].
Narrow diameters and fracture/early failure risk
Most implants in this series were 2.5–3.0 mm, a known risk domain for zirconia. The 2023 meta-analysis identified implant fracture and early failures as more frequent in narrow zirconia implants [1]. Design-outcome reviews similarly highlight diameter and connection geometry as major determinants of reliability [4]. The clustering of failures in posterior lower right sites—high load regions—supports this risk model.
Biology and soft-tissue advantages
Although quantitative MBL was not recorded, clinical soft-tissue stability and low inflammation were consistent with zirconia’s favorable mucosal response and low plaque affinity reported in clinical cohorts and reviews [3,7,8]. Patient-reported benefits of zirconia include high satisfaction with esthetics and function [7].
Zirconia in irradiated jaws
Seven implants were placed in post-radiotherapy jaws. Five remained stable in Patient R2, while two failed due to failure of integration between fibula bone and native jaw bone as in the case of Patient R1. Implant survival in head-and-neck oncology patients depends strongly on vascularity, dose, mucosal status, and reconstruction biology, irrespective of material [9,10]. Published oncology implant series show survival often around 90–93% at 5 years, with failures concentrated in heavily irradiated or reconstructed segments [9,10]. Our findings suggest zirconia can integrate in irradiated bone when local conditions are favourable, but reconstructed irradiated mandibles remain high-risk environments.
Torque and osteotomy strategy
This series used a ceramic-specific torque protocol (machine 15 Ncm, manual ≥25 Ncm). Literature emphasizes avoiding excessive torque with zirconia; primary stability relies on condensation-based osteotomy rather than titanium-style high-compression seating [4,11]. This protocol likely contributed to stable outcomes in the majority of cases.
Limitations
- Retrospective design and modest sample size.
- No quantitative MBL measurements; radiographs were reviewed qualitatively only.
- Incomplete demographic variables.
- Case-mix skewed toward posterior mandible and narrow diameters.
Future prospective work should include standardized bone-level tracking, PROMs, and stratification by diameter and host-bone risk.
Conclusion
Roughened single-piece zirconia implants placed with a condensation-respecting osteotomy and controlled torque demonstrated acceptable clinical survival and strong biological/aesthetic behavior over 6 months to 5 years. Outcomes align with contemporary evidence supporting one-piece zirconia systems as a viable alternative to titanium, especially in esthetic zones. Failures were confined to posterior mandibular high-load and reconstructed irradiated bone, emphasizing the primacy of host factors and diameter-related risk [1,4,6]. Zirconia implants may be considered for selected post-radiotherapy cases when vascularity and local bone biology are favorable.
Clinical Significance
- Zirconia implants offer metal-free esthetics, improved mucosal integration, and low plaque affinity [1,3,7].
- One-piece roughened zirconia systems show the most predictable survival in current evidence [1,6].
- Controlled, lower-torque insertion (15 Ncm machine → ≥25 Ncm hand finish) leverages bone condensation and reduces ceramic stress [4,11].
- Zirconia can remain stable in selected irradiated jaws, but reconstructed irradiated mandibles carry higher failure risk [9,10].
Figure 7: 5 zirconia implants placed in the 2nd and 3rd quadrant.
Table
| Patient ID | Age group | Gender | No of Implants | Regions treated | Diameters used (mm) | Length groups used | # failures | Failure reasons |
| P01 | 70+ | M | 6 | Lower Front, Lower Right | 3 | 10–15, 15–20 | 0 | — |
| P02 | 50+ | F | 2 | Lower Right | 2.5, 3.0 | 15–20 | 0 | — |
| P03 | 60+ | F | 2 | Lower Left | 2.5, 3.5 | >20 | 0 | — |
| P04 | 40+ | F | 6 | Lower Left, Lower Right | 2.5 | 15–20 | 0 | — |
| P05 | 60+ | M | 1 | Lower Right | 4 | >20 | 0 | — |
| P06 | 60+ | F | 1 | Lower Right | 3 | 15–20 | 1 | High load |
| P07 | 60+ | F | 1 | Upper Left | 3 | 15–20 | 0 | — |
| P08 | 50+ | F | 2 | Lower Left | 2.5 | 15–20 | 0 | — |
| P09 | 60+ | F | 1 | Lower Left | 4 | 15–20 | 0 | — |
| P10 | 60+ | F | 1 | Upper Right | 2.5 | >20 | 0 | — |
| P11 | 60+ | F | 1 | Lower Right | 2.5 | 15–20 | 1 | High load |
| P12 | 60+ | F | 1 | Upper Right | 3.5 | >20 | 0 | Not included in study due to less than 6 months of follow up |
| R1 | 50+ | F | 2 | Lower Right | 2.5 | >20 | 2 | Fibula failure (reconstructed segment) |
| R2 | 70+ | M | 5 | Lower Left, Upper Left | 2.5 | 15–20, >20 | 0 | — |
Declarations
Ethical approval
This retrospective case series was conducted in accordance with the Declaration of Helsinki. All data were anonymized prior to analysis. Formal ethics committee approval was not required for retrospective anonymized observational reporting as per institutional policy.
Informed consent
Written informed consent for treatment was obtained from all patients. Consent for use of anonymized clinical images will be obtained for publication.
Conflicts of interest
None declared.
Funding
No external funding.
References
- Mohseni P, et al. (2023). Clinical outcomes of zirconia implants: a systematic review and meta-analysis. Clin Oral Investig.
Publisher | Google Scholor - Jennes ME, et al. (2023). Prospective clinical study to evaluate the success and survival of two-piece zirconia implants: 12-month results. Int J Implant Dent
Publisher | Google Scholor - Roehling S, et al. (2023). Clinical and radiographic outcomes of zirconia dental implants after 5 years of loading: systematic review/meta-analysis. Clin Oral Implants Res.
Publisher | Google Scholor - Gul A, et al. (2024). Zirconia dental implants: relationship between design and clinical outcomes. J Dent.
Publisher | Google Scholor - Gargallo-Albiol J, et al. (2022). Clinical and radiographic outcomes of one-piece rough-surface zirconia implants: case series. Materials.
Publisher | Google Scholor - Morton D, et al. (2018). ITI Consensus 2018: Prosthodontics and implant dentistry — recommendations on zirconia implants. Clin Oral Implants Res.
Publisher | Google Scholor - Arefnia B, et al. (2025). Patient-reported outcomes of zirconia dental implants: systematic review. J Prosthodont Res.
Publisher | Google Scholor - Borgonovo AE, et al. (2021). Clinical and radiographic evaluation of zirconia implants: long-term outcomes. J Clin Med.
Publisher | Google Scholor - Curi MM, et al. (2018). Long-term success of dental implants in head-and-neck cancer patients: influence of radiotherapy. Oral Oncol.
Publisher | Google Scholor - Zuercher AN, et al. (2024). Clinical, radiographic and patient-reported outcomes of zirconia vs titanium implants: comparative cohort. Clin Oral Implants Res.
Publisher | Google Scholor - Hashim D, et al. (2016). Clinical survival of zirconia implants: systematic review. Clin Oral Investig.
Publisher | Google Scholor - Pjetursson BE, et al. (2018). ITI Consensus 2018 systematic review of implant restorations and complications. Clin Oral Implants Res.
Publisher | Google Scholor - Sterzenbach G, et al. (2025). RCT comparing 3-year outcomes of zirconia vs titanium implants. Clin Oral Investig.
Publisher | Google Scholor