Case Report
A Case of Carotid Tumour: Rare Presentation with Review
1Chief Consultant Surgeon, Aarvy Healthcare Superspeciality Hospital, Gurugram, Haryana, India.
2Aarvy Healthcare Superspeciality Hospital, Gurugram, Haryana, India.
3Medical Officer, Aarvy Healthcare Superspeciality Hospital, Gurugram, Haryana, India.
4Faculty DNB Surgery, Aarvy Healthcare Superspeciality Hospital, Gurugram, Haryana, India.
*Corresponding Author: Vikram Yadav, Chief Consultant Surgeon, Aarvy Healthcare Superspeciality Hospital, Gurugram, Haryana, India.
Citation: Yadav V, Gupta N, Rao A, Goyal S. (2025). A Case of Carotid Tumour: Rare Presentation with Review, Clinical Case Reports and Studies, BioRes Scientia Publishers. 10(6):1-5. DOI: 10.59657/2837-2565.brs.25.280
Copyright: © 2025 Vikram Yadav, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: September 25, 2025 | Accepted: October 09, 2025 | Published: October 16, 2025
Abstract
Carotid body tumour (CBT) is an uncommon hyper vascular tumour in the region of the head and neck. It develops from neural crest origin paraganglionic tissue. It presents as a slow-growing mass at the carotid bifurcation at the level of the upper border of the thyroid cartilage. Because of the high rate of neurovascular complications, resection of this tumour is challenging for surgeons. Preoperative embolization is considered for tumour over five cms (shambling class III), but it is not a routine as it carries risk. Early tumour detection is important for the successful management of these tumours. A case of CBT in a 45-year-old lady managed at our centre is being reported here, along with a recent review of the literature.
Keywords: carotid body tumour; carotid bifurcation; neurovascular complications
Introduction
The carotid body arises from the neural crest and plays a crucial role in the body's acute adaptation to fluctuations in oxygen, carbon dioxide, and pH concentrations. The carotid body protects the organs from hypoxic damage by releasing neurotransmitters that increase the ventilatory rate in response to stimulation [1]. A family of tumours of sympathetic and parasympathetic paraganglioma comprises paraganglioma. CBTs are uncommon neoplasms originating from neural crest-derived paraganglionic tissue at the carotid bifurcation. Von Haller described the carotid body tumour in 1743. The incidence of carotid body tumours (CBTs) is less than 1 in 30000. CBTs represent more than half of neck paragangliomas (PGLs) and arise from the neural crest [1]. It is uncommon before the age of 20 [2]. These tumours are more common in females than in males (1.9:1), but some Asian centres have reported the opposite [3]. The mechanisms of carotid body tumour formation are not known [4]. CBT is one of the most commonly encountered jugular paragangliomas that involve the carotid body chemoreceptors [5]. It is highly vascular in nature and can infiltrate the carotid bifurcation, compress cranial nerves, and extend to the skull base [5]. CBTs are so uncommon that their management recommendations are not easy [6]. Most of CBTs are benign, but a small percentage are malignant, and some can be functional, secreting catecholamines which can cause symptoms like hypertension and tachycardia, requiring alpha and beta-blockers. Early diagnosis and intervention are ideal for the best prognosis. Surgical excision is the gold standard for management. However, External Beam Radiotherapy may be needed for a large-sized tumour or recurrent cases. There is no fixed management protocol, as tumours are uncommon and individual surgeons or single institutions cannot accumulate a sufficient number of cases [7]. An attempt was made to predict the difficulties encountered during resection and the treatment outcome at our institution by reviewing our experience with this rare disease.
Case Report
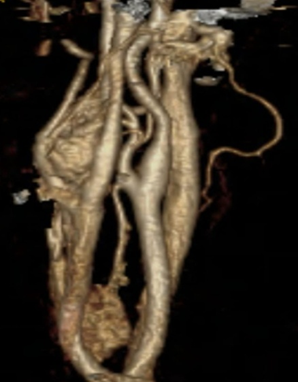
A 45-year-old presented with a history of vertigo with neck movement. On examination, there was no palpable lump. Doppler ultrasonography of the neck revealed a well-defined, hypoechoic, highly vascular mass at the bifurcation of the common carotid artery, without luminal compromise. CT angiography demonstrated a 3 cm carotid tumour [Figure 1]. There was a significant narrowing of the left carotid artery with neck movement.
Figure 1: CT angiography demonstrated a 3 cm carotid tumour.
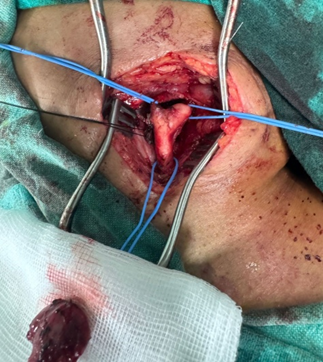
The neck was explored by a vertical incision under general anaesthesia. A homogeneous tumour about 4 x 3 cm long was present at the carotid bifurcation. It was classified as a grade-2 tumour according to the Shamblin classification system. The common carotid with internal and external arteries were isolated. Excision of a fairly vascular tumour at the bifurcation was possible. Ligation of small arterial branches arising from the bifurcation was carried out [Figure 2].
Figure 2: Removed Tumour.
Histologically, the tumour consisted of composed nests of uniform epithelioid cells with finely granular, pale eosinophilic cytoplasm and round nuclei, surrounded by a vascular stroma.
Discussion
Swiss Albrecht von Haller first described the carotid body in 1743, and the first descriptions of surgical excision of CBT are attributed to Marchand in 1891 and Scudder in 1903 [8].
The carotid body is a small, ovoid, pinkish-tan tissue situated in the peri-adventitia along the medial aspect of the carotid bifurcation bilaterally. It is a chemoreceptor that protects organs from hypoxic damage by releasing neurotransmitters to stabilize concentrations of oxygen, carbon dioxide, and pH [9].
CBTs are The incidence of CBTs is about 0.003% [10]; however, they represent 65% of head and neck paragangliomas (PGs) [11]. They occur at any age, but the mean patient age is 30-40 years, with a higher incidence in women [12]. Carotid body tumours can be bilateral in 5% of sporadic cases and in 33% of familial cases. Sporadic PGLs are multifocal in only 10% to 20% of cases; however, in familial cases, up to 80% are multifocal. Germline mutations cause familial cases of PGL in three of the four succinate dehydrogenase (SDH) subunit genes-SDHB, SDHC, and SDHD [13]. The early and complete surgical excision is mandatory due to the possibility of malignancy [14].
Most CBT patients present with a slow-growing (at rates of 0.5 cm per year), painless, compressible mass in the carotid triangle of the neck for several months. Local neck discomfort, pharyngeal swelling, headache, dizziness, dysphagia, tinnitus, hearing loss, voice change and transient ischemic attack (rarely) are other presenting symptoms. Preoperative cranial nerve deficit is uncommon. They have been reported in 0–20% of cases, and when present, the Vagus nerve is the most common among the lower cranial nerves to be involved [15].
On examination, the neck mass is mobile from side to side but less mobile in the craniocaudal direction due to adherence to the carotid arteries (Fontaine's sign). The mass is frequently pulsatile, and a bruit can be auscultated over the mass. They are usually located at the level of the tip of the hyoid bone at the anterior border of the sternocleidomastoid muscle. They may bulge into the pharynx or extend upward into the parapharyngeal space. The oral cavity should be carefully inspected as large PGs can fill the parapharyngeal space and displace the oropharyngeal wall medially.
If the PG is secretory, the most common finding is hypertension, which can be paroxysmal (lasting minutes to days) or sustained. Patients who only experience hypertensive paroxysms can be overlooked by a casual blood pressure measurement that is normal. Headache, palpitations, and sweating often accompany hypertension. Therefore, a careful history should be obtained from patients regarding any episodic symptoms, including frequency, duration, and any records of blood pressure and heart rate during the episodes.
Shamblin Classification
On preoperative MR imaging, a tumour-ICA (Internal Carotid Artery) maximum degree of circumference of contact less than or equal to 1800 would represent Shamblin I, circumferential contact more than 180 degrees and less than 270 degrees would represent Shamblin II, and greater than or equal to 270 degrees would represent Shamblin III.
Differential diagnoses of carotid body tumours include lymphedema, dermoid, brachial epidermoid, lipoma, pheochromocytoma, and neurofibroma.
Duplex US, CT, MRI, MRA, and DSA are used to diagnose suspected CBT. DSA is the gold standard in CBTs [16] for analyzing and planning treatment. DSA confirms the patency of the Circle of Willis and identifies feeding vessels to the tumour. And identifies other paragangliomas in the head and neck region. DSA can also determine the dominant. Feeding vessel, thereby allowing for preoperative embolization [17,18].
Colour-coded ultrasonography (CCU) enables the early and non-invasive, accurate detection of tumours with 100% sensitivity, even when they are not palpable [19]. The combined use of CCU and somatostatin receptor scintigraphy, including planar and single-photon emission computed tomography (SPECT), was found to be beneficial in identifying the extent of tumours and the degree of arterial infiltration. CT and MRI scans show infiltration in the neck and between the vessels. MRA is more preferable than MRI, as it provides both images of the tumour and data on vascular involvement [17,18,20].
The carotid body may lie in the carotid bifurcation or in the peri-adventitial plane [21]. Farr agrees with early resection of CBTs as this might avoid carotid artery resection, since the tumour grows somewhat loosely attached to the arterial wall and would thus be easier to detach at an early stage [22].
Vascular reconstruction is a common procedure and typically does not result in complications. Vascular resection and reconstruction were inevitable in a few cases. The rate of vascular repair in the literature ranges between 20% and 24% [20,21]. The incidence of cranial nerve injury was 10.71% but only 3.57% were permanent. Makaieff et al reported that the incidence of cranial nerve injury and stroke was 14.03%. Tumours larger than 4 cm were associated with a higher risk during removal. Early detection of smaller tumours should reduce the morbidity associated with the procedure [23].
Surgical approaches can be Trans-cervical, Trans-cervical with mandibulotomy and Trans-cervical with Trans-temporal for extension to the skull base, done under GA. It is recommended to collaborate with a vascular surgeon in nearly all cases. Excision of the tumour requires adequate exposure, as well as proximal and distal vascular control. Associated cranial nerves should be identified away from the lesion and dissected free. It is easiest to approach through the periadventitial avascular space between the vessels of the carotid system and the tumour [24]. The size of the tumour, the cranial extent of resection, and the Shamblin classification determine the occurrence of complications during surgery.
Radiation therapy is employed in patients who are poor candidates for surgical excision, due to the extent of the lesion, age or co-morbid conditions. The complications of radiotherapy include inflammation of the external auditory canal and middle ear, osteoradionecrosis, cranial nerve neuropathies, and direct injury to the brain tissue. Radiotherapy causes fibrosis resulting in difficulties in subsequent head and neck surgeries [25]. After surgery or radiotherapy, PGs with sporadic and familial occurrences require follow-up [26]. The malignancy rate of carotid PGs is estimated to be between 2 and 10%. Malignancy and multifocality are more common in familial paragangliomas [27].
Makeieff et al. and Qin et al. reported that routine preoperative embolisation is not required and should be limited to unresectable tumours to prevent disease progression [23,28]. The reason for this is that embolisation has its own risks, including an associated inflammatory response that makes precise periadventitial dissection more difficult [29] and the risk of intracranial embolisation [23]. Additionally, the probability of vascular repair is not ruled out [30]. Currently, embolisation is recommended only for tumours larger than 5 cm in size, Shamblin’s class III, and those located cranially [31]. A covered stent can be inserted in the external carotid artery as an alternative to embolisation [32].
Conclusion
The accurate and early diagnosis of CBTs is crucial for performing successful surgery. The latest diagnostic tools are very useful for early detection. Vascular reconstructions can be done safely without serious complications.
References
- Wieneke, J. A., Smith, A. (2009). Paraganglioma: carotid body tumor. Head and Neck Pathology, 3(4):303-306.
Publisher | Google Scholor - Mendenhall, W., Werning, J., Peister, D. (2011). Treatment of head and neck cancer (paragangliomas). Cancer: Principles and Practice of Oncology, 9th ed. Philadelphia: Lippincott, 722-723.
Publisher | Google Scholor - Nazari, I., Moghaddam, F. A., Zamani, M. M., Salimi, J. (2012). Clinical characteristics and remedies in 45 Iranians with carotid body tumors. Acta Medica Iranica, 339-343.
Publisher | Google Scholor - Kay, J. M., Laidler, P. (1977). Hypoxia and the carotid body. Journal of Clinical Pathology. Supplement (Royal College of Pathologists), 11:30.
Publisher | Google Scholor - Ma, D., Liu, L., Yao, H., Hu, Y., Ji, T., et al. (2009). A retrospective study in management of carotid body tumour. British Journal of Oral and Maxillofacial Surgery, 47(6):461-465.
Publisher | Google Scholor - Knight Jr, T. T., Gonzalez, J. A., Rary, J. M., Rush, D. S. (2006). Current concepts for the surgical management of carotid body tumor. The American Journal of Surgery, 191(1):104-110.
Publisher | Google Scholor - Maxwell, J. G., Jones, S. W., Wilson, E., Kotwall, C. A., Hall, T., et al. (2004). Carotid body tumor excisions: adverse outcomes of adding carotid endarterectomy. Journal of the American College of Surgeons, 198(1):36-41.
Publisher | Google Scholor - Zbaren, P., Lehmann, W. (1985). Carotid body paraganglioma with metastases. The Laryngoscope, 95(4):450-454.
Publisher | Google Scholor - Naughton, J., Morley, E., Chan, D., Fong, Y., Bosanquet, D., et al. (2011). Carotid body tumours. British Journal of Hospital Medicine, 72(10):559-564.
Publisher | Google Scholor - Gad, A., Sayed, A., Elwan, H., Fouad, F. M., Eldin, H. K., et al. (2014). Carotid body tumors: a review of 25 years’ experience in diagnosis and management of 56 tumors. Annals of Vascular Diseases, 7(3):292-299.
Publisher | Google Scholor - Georgiadis, G. S., Lazarides, M. K., Tsalkidis, A., Argyropoulou, P., Giatromanolaki, A. (2008). Carotid body tumor in a 13-year-old child: Case report and review of the literature. Journal of Vascular Surgery, 47(4):874-880.
Publisher | Google Scholor - Ward, P. H., Jenkins, H. A., Hanafee, W. N. (1978). Diagnosis and treatment of carotid body tumors. Annals of Otology, Rhinology & Laryngology, 87(5):614-621.
Publisher | Google Scholor - Fruhmann, J., Geigl, J. B., Konstantiniuk, P., Cohnert, T. U. (2013). Paraganglioma of the carotid body: treatment strategy and SDH-gene mutations. European Journal of Vascular and Endovascular Surgery, 45(5):431-436.
Publisher | Google Scholor - Smith, J. J., Passman, M. A., Dattilo, J. B., Guzman, R. J., Naslund, T. C., et al. (2006). Carotid body tumor resection: does the need for vascular reconstruction worsen outcome? Annals of Vascular Surgery, 20(4):435-439.
Publisher | Google Scholor - Pellitteri, P. K., Rinaldo, A., Myssiorek, D., Jackson, C. G., Bradley, P. J., et al. (2004). Paragangliomas of the head and neck. Oral Oncology, 40(6):563-575.
Publisher | Google Scholor - Ma, D., Liu, M., Yang, H., Ma, X., Zhang, C. (2010). Diagnosis and surgical treatment of carotid body tumor: A report of 18 cases. Journal of Cardiovascular Disease Research, 1(3):122-124.
Publisher | Google Scholor - Luna-Ortiz, K., Rascon-Ortiz, M., Villavicencio-Valencia, V., Granados-Garcia, M., Herrera-Gomez, A. (2005). Carotid body tumors: review of a 20-year experience. Oral Oncology, 41(1):56-61.
Publisher | Google Scholor - Sajid, M. S., Hamilton, G., Baker, D. M. (2007). A multicenter review of carotid body tumour management. European Journal of Vascular and Endovascular Surgery, 34(2):127-130.
Publisher | Google Scholor - Martinelli, O., Irace, L., Massa, R., Savelli, S., Giannoni, F., et al. (2009). Carotid body tumors: radioguided surgical approach. Journal of Experimental & Clinical Cancer Research, 28(1):148.
Publisher | Google Scholor - Ma, D., Liu, L., Yao, H., Hu, Y., Ji, T., et al. (2009). A retrospective study in management of carotid body tumour. British Journal of Oral and Maxillofacial Surgery, 47(6):461-465.
Publisher | Google Scholor - Kotelis, D., Rizos, T., Geisbüsch, P., Attigah, N., Ringleb, P., et al. (2009). Late outcome after surgical management of carotid body tumors from a 20-year single-center experience. Langenbeck's Archives of Surgery, 394(2):339-344.
Publisher | Google Scholor - Farr, H. W. (1980). Carotid body tumors: a 40-year study. CA: A Cancer Journal for Clinicians, 30(5):260-265.
Publisher | Google Scholor - Makeieff, M., Raingeard, I., Alric, P., Bonafe, A., Guerrier, B., et al. (2008). Surgical management of carotid body tumors. Annals of Surgical Oncology, 15(8):2180-2186.
Publisher | Google Scholor - Browse, N. L. (1982). Carotid body tumours. British Medical Journal (Clinical research ed.), 284(6328):1507.
Publisher | Google Scholor - Hinerman, R. W., Mendenhall, W. M., Amdur, R. J., Stringer, S. P., Antonelli, P. J., et al. (2001). Definitive radiotherapy in the management of chemodectomas arising in the temporal bone, carotid body, and glomus vagale. Head & Neck, 23(5):363-371.
Publisher | Google Scholor - Benn, D. E., Gimenez-Roqueplo, A. P., Reilly, J. R., Bertherat, J., Burgess, J., et al. (2006). Clinical presentation and penetrance of pheochromocytoma/paraganglioma syndromes. The Journal of Clinical Endocrinology & Metabolism, 91(3):827-836.
Publisher | Google Scholor - Papaspyrou, K., Mann, W. J., Amedee, R. G. (2009). Management of head and neck paragangliomas: review of 120 patients. Head & Neck, 31(3):381-387.
Publisher | Google Scholor - Qin, R. F., Shi, L. F., Liu, Y. P., Lei, D. L., Hu, K. J., et al. (2009). Diagnosis and surgical treatment of carotid body tumors: 25 years’ experience in China. International Journal of Oral and Maxillofacial Surgery, 38(7):713-718.
Publisher | Google Scholor - Netterville, J. L., Reilly, K. M., Robertson, D., Reiber, M. E., Armstrong, W. B., et al. (1995). Carotid body tumors: a review of 30 patients with 46 tumors. The Laryngoscope, 105(2):115-126.
Publisher | Google Scholor - Smith, J. J., Passman, M. A., Dattilo, J. B., Guzman, R. J., Naslund, T. C., et al. (2006). Carotid body tumor resection: does the need for vascular reconstruction worsen outcome? Annals of Vascular Surgery, 20(4):435-439.
Publisher | Google Scholor - Kakkos, S. K., Reddy, D. J., Shepard, A. D., Lin, J. C., Nypaver, T. J., et al. (2009). Contemporary presentation and evolution of management of neck paragangliomas. Journal of Vascular Surgery, 49(6):1365-1373.
Publisher | Google Scholor - Scanlon, J. M., Lustgarten, J. J., Karr, S. B., Cahan, J. I. (2008). Successful devascularization of carotid body tumors by covered stent placement in the external carotid artery. Journal of Vascular Surgery, 48(5):1322-1324.
Publisher | Google Scholor